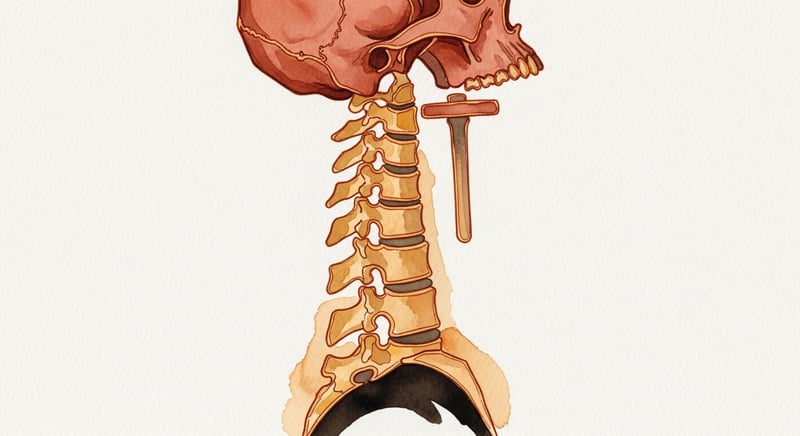
The Atlas-Axis Joint: The Most Loaded Joint in Your Neck
Key Takeaways
- The atlanto-axial joint sits between your first cervical vertebra (C1, the atlas) and your second (C2, the axis). It carries the full weight of your skull through a structure that is built nothing like the rest of your spine.
- C1 has no vertebral body and no spinous process. C2 has a vertical bony peg (the dens) that pokes up into C1 and acts as the rotation axis for your head.3
- The joint accounts for about half of all neck rotation and runs as a pivot, with the rest of your cervical spine handling flexion, extension, and lateral bend.1
- The transverse ligament is the strongest ligament in your cervical spine. It pins the dens in place. When it fails (rheumatoid arthritis, Down syndrome, or trauma), the resulting instability is a medical emergency.2
- If you have neck pain that radiates to the back of the head, a heavy-skull feeling at the end of long screen days, or rotation that has quietly become asymmetric, the upper cervical joint is the place to start looking.
Most posture conversations stop at the cervical curve as a single thing. The reality is that the top two vertebrae do not look or work like the rest. The atlanto-axial joint, the meeting point of your first and second cervical vertebrae, is the most mechanically peculiar segment in your spine. It carries the full weight of your skull, owns about half of your head rotation, and is held together by a single ligament that, when it fails, becomes a medical emergency. Knowing how this joint works changes how you think about neck tension, suboccipital headaches, and the upper-cervical mobility work that suddenly feels like it is doing more than the rest of the program combined.
Why this joint deserves its own post
Your cervical spine has seven vertebrae, but they are not seven copies of the same template. The bottom five (C3 through C7) follow the typical pattern: a vertebral body in front, a bony arch in back, a disc between each level, and roughly equal contributions to flexion, extension, side bend, and rotation. The top two are different. C1 has no body and no spinous process. C2 has a vertical peg that pokes up through C1's ring. There is no disc between them.
Together C1 and C2 form a system that does one job exceptionally well and the rest of the cervical spine cannot do at all: rotation. About half of your total neck rotation, the kind you use to check a blind spot in the car or follow a moving object across a room, happens at the atlanto-axial joint alone.1 The remaining cervical levels share the other half between them. Flexion and extension follow a different distribution: the atlanto-occipital joint above C1 (the joint between the skull and the atlas) handles most of the nodding motion, while C3 through C7 cover the rest.
This division of labor matters for two reasons. First, when one segment is restricted, the others have to compensate. Suboccipital tension and limited rotation almost always mean the upper-cervical joints are not doing their share, and the lower cervical levels are working overtime to give the impression of normal head movement. Second, the atlanto-axial joint is innervated mostly by the C2 spinal nerve, the same nerve that supplies the back of the scalp.1 That is why upper-cervical irritation often shows up as a dull pain at the base of the skull or a headache that wraps around to behind the eye.
If you have read the spinal-curves explainer or the forward-head guide, you have already met the cervical curve as a system. This post zooms in on the segment that does most of the work.
About half of your total neck rotation happens at one joint. The remaining cervical levels share the other half.

C1 and C2: built nothing like the rest of the spine
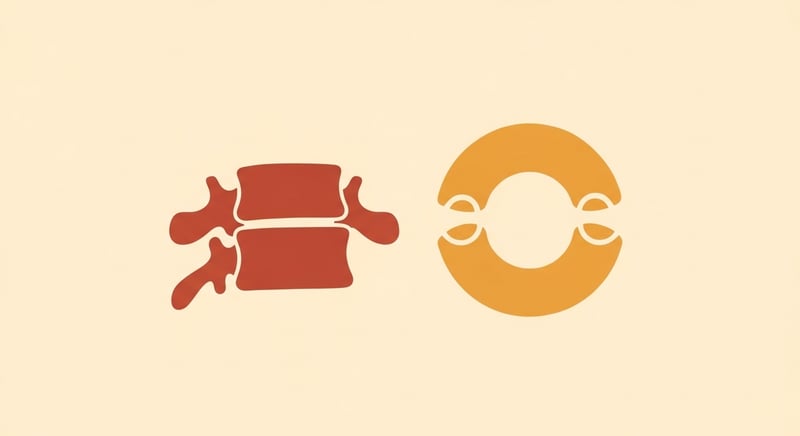
Pick up a model of a typical lumbar vertebra and you see the same recipe most of your spine follows: a thick disc-shaped body in front carries the weight, a bony ring behind it protects the spinal cord, and seven processes (one spinous, two transverse, four articular) stick out for muscle attachment and joint surfaces. C1 throws most of that out.
C1, the atlas (named after the Greek titan who held up the sky), is essentially a bony ring with two bulges on top and two on the bottom. The bulges are called lateral masses, and they take all the weight of your skull on the top side, then transfer it down to C2 on the bottom side. There is no body. There is no spinous process. There are no traditional articulating facets between C1 and C2 the way there are everywhere else in the spine. What there is, instead, is a complete absence of an intervertebral disc and a strange piece of vertical bone shooting up from C2.3
C2, the axis, has its name for that vertical bone. It is called the dens (Latin for tooth) or the odontoid process, and it is the most distinctive feature in the entire spine. The dens projects up from the body of C2, slips through the front of the C1 ring, and sits behind the front of C1's bony arch. Your skull and C1 then rotate around the dens like a ball turning on a peg. This is why the atlanto-axial joint is a pivot joint, the only one in the spine.3
The functional consequence of all this strange architecture is that C1-C2 has zero passive bony stability against rotation. There is no disc to pin the segments together, no traditional facets to lock the motion. The joint is held together entirely by ligaments. That is the trade-off the body made for rotation range: trade bony stability for ligamentous flexibility, then build a ridiculously strong ligament to keep the dens where it belongs.
The ligaments: how the dens stays where it should
Four named ligaments do the work of keeping C1, C2, and your skull in alignment. Three of them are interesting. One of them is structurally critical.1
The transverse ligament of the atlas is the headline. It is a thick band of fibrous tissue that runs horizontally across the inside of the C1 ring, behind the dens. Its job is to pin the dens to the front of the ring and prevent it from sliding backward into the spinal cord. The transverse ligament is the strongest single ligament in the entire cervical spine.2 When it does its job, the dens stays put and the rotation pivot works as designed.
The alar ligaments run from the top of the dens out to the inside of the skull at each side. They limit how far you can rotate your head before the dens engages and stops you. If you have ever felt your head reach a clear endpoint when you turn it as far as it will go, those are your alar ligaments saying enough.
The apical ligament of the dens runs from the very top of the dens up to the front rim of the foramen magnum (the hole in the base of your skull where the spinal cord exits). It is small and not particularly load-bearing on its own. It mostly contributes to the overall stability of the dens-to-skull connection.
The tectorial membrane is a broad sheet of tissue, essentially a continuation of the posterior longitudinal ligament from the rest of the spine, that drapes over the back of the dens and attaches to the inside of the skull. It contributes to overall stiffness of the upper cervical complex.
If the transverse ligament fails, the dens loses its anchor. With every flexion of the head it can shift backward into the spinal cord, which is sitting one or two millimeters away. This is the central injury in atlanto-axial instability. About 30% of people with Down syndrome have radiographic atlanto-axial instability (though only about 1% are symptomatic), and 25 to 80 percent of people with long-standing rheumatoid arthritis develop some degree of upper-cervical involvement, primarily through inflammatory erosion of the transverse ligament.2 In trauma the same ligament can rupture from a high-speed flexion injury. All of these are medical emergencies and are not the kind of thing posture work alone fixes.
The transverse ligament is the strongest single ligament in your cervical spine. It is also the only thing keeping the dens from drifting into your spinal cord.
Suboccipital muscles: why upper-cervical tension feels different
Sitting in the small triangular space between your skull, C1, and C2 are four pairs of small muscles called the suboccipital group. They are the rectus capitis posterior major, rectus capitis posterior minor, obliquus capitis superior, and obliquus capitis inferior. They are tiny compared to the trapezius and the levator scapulae, but their density of muscle spindles (the sensory organs that tell your brain where a muscle is in space) is among the highest of any muscle in the body.
The function of the suboccipital group is precise micro-movement of the skull on the upper cervical spine and continuous postural correction.1 When you tilt your head a few millimeters to follow a slow-moving object, the suboccipitals fire. When you compensate for a tiny shift in standing balance, the suboccipitals fire. They never really stop working, which is part of why they accumulate tension across a day in a way that bigger postural muscles do not.
The clinical consequence is that suboccipital tension feels different from regular neck tension. People describe it as a dull pressure or band sensation at the base of the skull rather than a sharp pain. It often refers up into the head as a tension-type headache that wraps around to behind the eye, because the C2 nerve that innervates the upper cervical joint also supplies the back and crown of the scalp.1 Tension headaches and upper cervical tightness are mechanistically the same problem viewed from two angles.
The standard at-home reset is the chin tuck. Done correctly, it lengthens the suboccipital muscles, improves the position of the skull on C1, and restores upper-cervical extension that hours of looking down at screens has compressed away. The full chin-tuck protocol is in the chin tucks exercise guide and the deeper neck-pain routine in the neck pain relief exercises post. Both are designed around the upper cervical mechanics this post just walked through.

What this means for your posture practice
Three practical takeaways from the anatomy.
First, upper-cervical mobility is not the same as general neck stretching. When the suboccipitals are tight and the C1-C2 joint is restricted, no amount of full-neck side bend or general trapezius stretching restores the lost rotation. The work has to be specific to the upper cervical region: chin tucks, gentle upper-cervical extension over a rolled towel, careful head-rotation drills that isolate the C1-C2 segment without engaging the lower cervical levels. The first ten degrees of rotation in either direction are mostly C1-C2; if you cannot get them, the problem is likely upper, not lower.
Second, your head position over the rest of your spine is decided more by C1-C2 than by C3-C7. The atlas and axis are the segments closest to the skull, so any restriction or tilt at that level translates directly into how your head sits on your neck. This is why forward-head posture often improves more from upper-cervical work than from middle-or-lower cervical stretching, even though the visible problem looks like it spans the whole neck. The forward head posture guide covers the full chain; this post is the upstream piece.
Third, screen habits load this joint differently than the rest. When you look down at a phone, the lower cervical spine does most of the visible flexion. But to keep your eyes level with the screen rather than pointed at the floor, the suboccipitals at C1-C2 have to extend to compensate. Over a day this asymmetric loading (lower cervical flexion + upper cervical extension) is what produces the dull-pressure tension at the base of the skull that so many phone-heavy users describe. The text neck syndrome post walks through the screen-time mechanics in more detail.
If your neck tension lives at the base of your skull rather than across the shoulders, if your head rotation is asymmetric, or if you get tension headaches that wrap around to behind the eye, treat the upper cervical joint as the primary suspect and adjust your practice accordingly.
When to see a professional
The work in this post is appropriate for healthy adults with everyday neck tension. If any of the following apply to you, talk to a clinician before starting upper-cervical mobility drills.
See a doctor if you have rheumatoid arthritis, Down syndrome, or skeletal dysplasia. All three are associated with significantly elevated rates of atlanto-axial instability through different mechanisms, and head rotation drills can be unsafe without imaging-guided supervision.2
See a doctor if you have had a recent high-speed flexion injury (motor-vehicle collision, fall onto the head, sports impact), especially if you have any new neurological symptoms (tingling in the hands, weakness, balance changes). Trauma to the transverse ligament is a serious diagnosis that requires imaging.
See a doctor for any sudden onset of severe headache, balance loss, slurred speech, or visual disturbance associated with neck movement. The vertebral arteries pass through the transverse foramina of C1 and C2 on their way to the brainstem.1 Forceful upper-cervical manipulation in the wrong setting (typically high-velocity rotational thrust without prior screening) carries a small but real risk of vertebral artery dissection. Self-directed gentle mobility work is not the same as a high-velocity manipulation, but the awareness is worth carrying.
For everyone else, the upper-cervical region rewards the same patient daily attention any other postural segment does.
If your neck tension lives at the base of your skull rather than across the shoulders, treat the upper cervical joint as the primary suspect.
Frequently Asked Questions
Why does my neck pain wrap around to behind my eye?
The C2 spinal nerve innervates the upper cervical joint and also supplies the back and top of your scalp. Irritation at the atlanto-axial joint or in the suboccipital muscles can refer pain along the C2 distribution, which often presents as a tension headache that starts at the base of the skull and wraps over the head to behind the eye.1
Are chin tucks really enough to fix upper-cervical tension?
For everyday tension from screen use and habitual forward-head positioning, yes, when done consistently. Chin tucks lengthen the suboccipital muscles and restore upper-cervical extension that screen time compresses away. The full progression is in the chin tucks exercise guide. For tension that does not respond to four weeks of consistent practice, a manual therapist or physical therapist can address joint-level restrictions that home work cannot reach.
What is the difference between the atlanto-occipital joint and the atlanto-axial joint?
The atlanto-occipital joint is between your skull (the occipital bone) and C1, the atlas. It handles most of your head's nodding motion. The atlanto-axial joint is between C1 and C2, the axis. It handles most of your head's rotation. Both are part of the upper cervical complex, but they do different jobs and respond to slightly different mobility work.
Can I crack my own neck safely?
Self-applied gentle stretching that produces a small audible release at the base of the neck is generally safe for healthy adults. What is not safe is forceful rotational manipulation of the upper cervical region, which carries a small but real risk of vertebral artery dissection. If you feel the urge to crack your neck constantly, that is usually a signal that the joint is restricted and would benefit from gentle daily mobility work rather than a single hard release.
Is the dens what people mean by hangman's fracture?
Closely related but not the same. A hangman's fracture is a fracture of the pars interarticularis of C2, typically from hyperextension trauma. A dens fracture (also called an odontoid fracture) is a separate injury in which the dens itself breaks. Both are serious cervical injuries that require imaging and specialist care.