Lower Back Pain from Poor Posture: Causes and Solutions
Key Takeaways
- Slumping in your chair roughly doubles the pressure on your lower-back discs compared to standing tall.
- Two slouch patterns drive most desk-job back pain: flat back (pelvis tucked under) and over-arched back (pelvis tipped forward).
- Moving matters more than sitting "right." Get up every 30 to 45 minutes and your back will thank you.
- Crunches make a sore lower back worse. Train deep core muscles with planks and dead-bugs instead.
- Most posture-driven back pain eases within two to four weeks of the right exercises. If yours doesn't, see someone.
Lower back pain caused by poor posture is a mechanical problem. When the lumbar spine sits out of its natural curve for hours a day, the muscles, discs, and ligaments that support it absorb loads they were not built for. Sitting with a rounded back flattens the lumbar curve and pushes disc pressure up. Standing with an exaggerated arch compresses the facet joints. Both patterns cause pain, and both are fixable with the right exercises and habit changes.
We see this pattern regularly in the research we review at UpWise. Lower back pain is the leading cause of disability worldwide, affecting an estimated 619 million people in 2020 according to the Global Burden of Disease study.1 And while not all back pain is postural, a large proportion of the chronic, non-specific variety is directly tied to how people sit, stand, and move through their day. The good news: postural back pain is among the most responsive to conservative treatment.
Why Poor Posture Causes Lower Back Pain
The lumbar spine has a natural lordotic curve, a gentle forward arc that distributes your body weight evenly across the five lumbar vertebrae and their discs. When that curve is maintained, each disc bears a roughly equal share of the load. When the curve is flattened or exaggerated, the load shifts.
Wilke et al. (1999) published what remains one of the most-cited studies on spinal loading. Using pressure sensors implanted in the L4-L5 disc of a volunteer, they found that sitting in a slouched position increased intradiscal pressure by approximately 40% compared to relaxed standing. Sitting while leaning forward, the posture most people adopt at a desk, increased it further.2 That increased pressure is not dangerous for five minutes. It becomes a problem over hours, days, and months.
Over time, sustained uneven loading weakens the annulus fibrosus, the tough outer ring of the disc. The disc loses hydration. The gel-like nucleus inside can shift toward the weakened side. This is the mechanism behind disc bulges and herniations, and it starts with nothing more dramatic than sitting badly for too long. For a broader look at the relationship between back pain and posture, our back pain and posture guide covers the full picture.
Which Posture Types Cause It
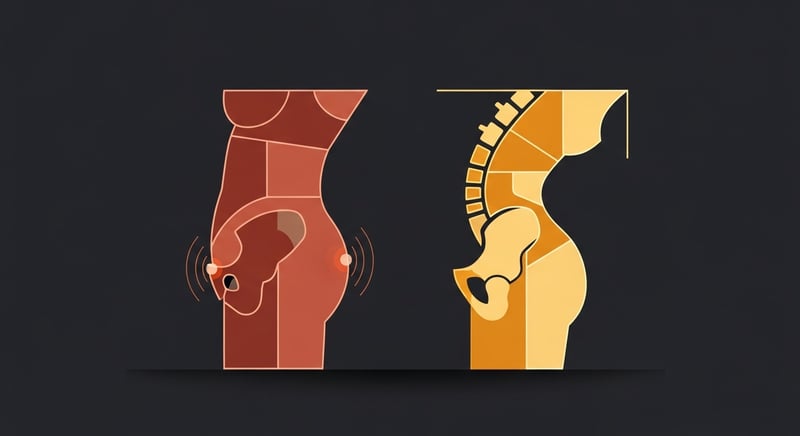
Not all poor posture creates lower back pain. The two types most strongly associated with lumbar problems are posterior pelvic tilt (flat back posture) and anterior pelvic tilt (excessive lordosis).
Posterior pelvic tilt happens when the pelvis rotates backward, flattening the lumbar curve. This is what most desk workers develop. The hip flexors shorten from sitting, the hamstrings tighten, and the glutes weaken. The result: the pelvis tucks under, the lower back flattens, and disc pressure increases because the spine has lost its shock-absorbing curve. People with flat back posture tend to feel a dull ache across the lower back that worsens after long periods of sitting.
Anterior pelvic tilt is the opposite pattern. The pelvis tips forward, increasing the lumbar arch. Tight hip flexors (especially the iliopsoas) and weak abdominals are the usual culprits. The excessive curve compresses the facet joints in the lumbar spine, small paired joints on the back of each vertebra. Facet joint irritation tends to produce a sharper pain, often on one side, that worsens with standing and extension.
A 2014 study in Manual Therapy found that people with chronic lower back pain were significantly more likely to have either excessive or reduced lumbar lordosis compared to pain-free controls.3 The study is not saying that everyone with a curved or flat back will develop pain. It is saying the odds increase when the curve drifts far enough from neutral in either direction.
The Sitting Problem
Sitting gets most of the blame for lower back pain, and there is good reason for that. But the issue is not sitting itself. The issue is sitting the same way for hours without moving.
When we sit, the hip flexors shorten, the lumbar curve flattens, and the posterior ligaments of the spine stretch. All of this is fine in short doses. The body adapts to brief positional changes. Problems start when the position becomes chronic. A 2019 systematic review in the Journal of Orthopaedic and Sports Physical Therapy concluded that no single sitting posture has been proven to prevent back pain. What the evidence does support is regular movement breaks and positional variation.4
The practical takeaway: it is not about finding the perfect chair or the perfect sitting position. It is about not staying in any position long enough for tissue adaptation to occur. A good rule is to change positions every 30 to 45 minutes. Stand up. Walk to the kitchen. Do a 60-second stretch. Then sit back down. That interruption resets the loading cycle and gives your discs the compression-decompression cycle they need. If you spend most of your day at a desk, our guide to sitting in an office chair covers the adjustments that reduce lumbar load.

Exercises That Help
The exercise approach depends on which postural pattern is behind your pain. But there is one principle that applies to both: strengthen the deep stabilizers of the spine before adding load or range of motion.
The transverse abdominis and multifidus are the two muscles that matter most for lumbar stability. The transverse abdominis wraps around your torso like a corset and stiffens the spine from the front and sides. The multifidus runs along the vertebrae and controls segmental movement. Research by Hodges and Richardson (1996) showed that in people with lower back pain, these muscles activate late or not at all, leaving the spine unsupported during movement.5
Core strengthening for posture does not mean doing crunches. Crunches actually increase lumbar disc pressure and train the rectus abdominis (the "six-pack" muscle), which is not a primary spinal stabilizer. The exercises that work for postural back pain are bird dogs, dead bugs, pallof presses, and modified planks. These train the deep stabilizers in positions that do not load the spine.
For posterior pelvic tilt, add hip flexor stretches (kneeling lunge stretch, couch stretch) and glute bridges to reactivate the glutes. For anterior pelvic tilt, focus on the hip flexor stretches plus hamstring curls and posterior pelvic tilt exercises that teach the pelvis to rotate back to neutral.
Daily Habits for Relief
Exercise is half the equation. The other half is the 15 or so hours a day when you are not exercising. The habits you maintain during work, commuting, and relaxing determine whether the exercise gains stick or get erased by the end of the day.
Set a timer for 30-minute movement breaks during desk work. Stand up, walk for a minute or two, do a quick hip flexor stretch. This is the single most impactful habit change for posture-related back pain. The evidence on this is consistent: sustained static postures damage tissue, and regular breaks prevent the damage from accumulating.
When you do sit, keep the lumbar curve supported. A lumbar support cushion or even a rolled-up towel in the small of your back helps maintain the curve without relying on muscle effort alone. Adjust your chair so your hips sit slightly higher than your knees. This tilts the pelvis forward just enough to preserve the lumbar curve without forcing it.
Sleeping position matters too. Sleeping on your back with a pillow under your knees reduces lumbar extension. Sleeping on your side with a pillow between your knees keeps the pelvis aligned. Sleeping on your stomach is the worst position for the lower back because it forces the lumbar spine into extension for hours.
Walking is underrated. A daily 20 to 30 minute walk does more for lower back pain than most people expect. Walking gently loads and unloads the spinal structures in a rhythmic pattern that promotes disc nutrition, builds endurance in the postural muscles, and reduces the stiffness that accumulates from sitting. A Cochrane review found that walking programs were as effective as structured exercise programs for chronic lower back pain.6
Frequently Asked Questions
Can poor posture alone cause lower back pain?
Yes, though it is rarely the only factor. Sustained poor posture changes how load is distributed across the lumbar spine. Sitting with a rounded lower back flattens the natural lumbar curve and increases pressure on the intervertebral discs by 40 to 85 percent compared to standing. Over months and years, this creates tissue fatigue and pain. But other factors like activity level, stress, sleep, and body weight interact with posture to determine who actually develops symptoms.
How long does it take for posture changes to relieve lower back pain?
Most people notice a reduction in symptoms within 2 to 4 weeks of consistent corrective exercise and postural adjustments. Research shows that 8 weeks of targeted exercise produces measurable changes in spinal alignment. Full resolution of chronic pain takes longer, often 3 to 6 months. The key factor is consistency: doing the exercises daily and changing the sitting and standing habits that caused the problem.
Is sitting or standing worse for lower back pain?
Neither is inherently worse. What matters is how long you hold any single position. Sitting with a rounded back loads the lumbar discs unevenly. Standing in a swayback posture compresses the facet joints. The evidence points to movement variety as the most protective factor. Alternating between sitting, standing, and walking every 30 to 45 minutes reduces sustained load on any one structure.