
Piriformis Syndrome: The Sitting Posture Connection
Key Takeaways
- Piriformis syndrome is sciatic-type pain caused by the deep gluteal muscle compressing the sciatic nerve, not by a lumbar disc.
- It accounts for about 0.3 to 6 percent of all low-back-pain or sciatica cases, with female-to-male ratio about 6 to 1, and prolonged sitting is the most common trigger.
- Pain that worsens with sitting and improves with standing or walking, concentrated in the buttock with referral above the knee, points to piriformis rather than a disc.
- The optimized stretch position is 115 degrees of hip flexion, 40 degrees of external rotation, and 25 degrees of adduction. It elongates the muscle 30 to 40 percent versus 12 percent for conventional figure-four.
- Conservative treatment alone resolves about 41 percent of cases. Combined with procedures the overall success rate is around 93 percent.
Piriformis syndrome is a real condition with a specific mechanism, distinct from the sciatica most readers know. The piriformis is a small flat muscle deep in the glute, behind the hip joint, and the sciatic nerve runs right next to it. When the muscle gets irritated or tight, it presses against the nerve and creates the same buttock-and-leg pain a herniated disc produces. The key difference is location. Disc-related sciatica starts at the lower spine. Piriformis syndrome starts at the back of the hip. Most cases I have seen come from prolonged sitting in the same position, and the fix has to address both the muscle and the seated habit.
What the piriformis actually does
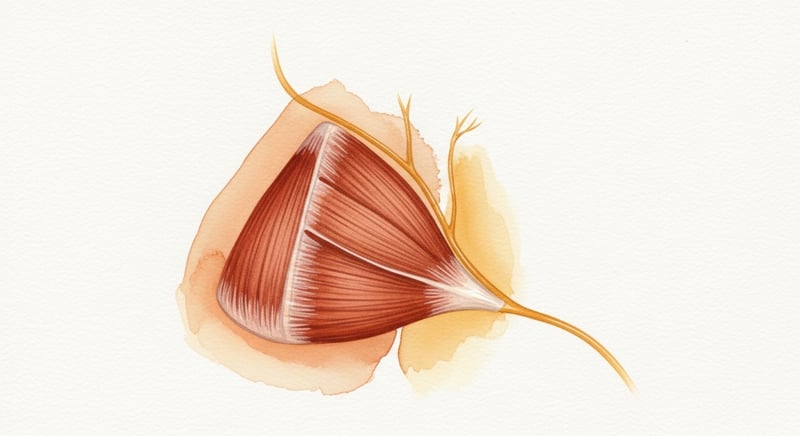
The piriformis is a flat, pyramidal muscle that runs from the front of the sacrum out to the top of the femur. Its job is to rotate the hip outward (external rotation) and to stabilize the pelvis when you stand on one leg. Most people never think about it because larger muscles like the glute max do similar work in obvious ways.
The clinically important detail is that the sciatic nerve runs immediately next to it as it exits the pelvis through the greater sciatic notch1. In most people the nerve passes underneath the piriformis. In a smaller fraction (estimated at around 20 percent across cadaver studies), the nerve passes through the muscle. This anatomical variation is part of why some people are more susceptible to compression than others.
When the muscle thickens, spasms, or shortens, the nerve gets squeezed against bone. The result is a deep ache in the buttock that can refer down the back of the thigh and sometimes all the way to the foot. Patients describe it as sitting on a tennis ball, which is a useful mental image for what is actually happening at the joint level.
Prevalence estimates put piriformis syndrome at 0.3 to 6 percent of all low-back-pain or sciatica cases, with women affected roughly six times more often than men1. The female prevalence is partly anatomical (wider pelvis, slightly different sciatic-nerve angle) and partly behavioral (different seated postures and footwear distributions over time).
Why prolonged sitting compresses it
Prolonged sitting is the most common piriformis trigger. The 2023 StatPearls entry lists taxi drivers, office workers, and bicycle riders as the typical patient profile, and recommends avoiding prolonged sitting with hourly breaks as a first-line measure1.
The mechanism is positional. When you sit with your knees lower than your hips and your thighs angled together (the standard slouched office posture), your hip drops into flexion plus internal rotation plus adduction. In that combined position the piriformis sits both stretched and compressed against the seat surface. Hold it for a few hours and the muscle responds by tightening. A tight piriformis presses harder against the sciatic nerve. The cycle repeats the next day.
A wallet in the back pocket makes it worse. So does a bicycle saddle that is too narrow or set at the wrong height. So does a low couch where your hips drop below your knees. The common thread is sustained pressure on the muscle from below combined with hip positioning that keeps it in a shortened state.
This is also why piriformis pain often shows up with hip pain from extended desk sitting, even though the two conditions have different mechanisms. The same prolonged-flexion habit that shortens the hip flexors also irritates the piriformis. People with one usually have at least mild signs of the other.
The piriformis sits both stretched and compressed against the seat surface in that position. Hold it for a few hours and the muscle responds by tightening.

How piriformis pain differs from spinal sciatica
The distinction matters because treatment is different. If your sciatic pain is coming from a herniated lumbar disc, the right response is positional unloading at the lumbar spine, and aggressive piriformis stretching can make it worse. If your sciatic pain is coming from the piriformis, lumbar treatment will not help much.
Three signals suggest piriformis as the source rather than a disc. First, the pain is worst with prolonged sitting and improves when you stand or walk. Disc pain often does the opposite (worse with prolonged standing, better seated with a slight forward lean). Second, the pain is concentrated in the buttock and may radiate down the back of the thigh, but rarely past the knee. Third, deep palpation directly into the piriformis (about midway between the sacrum and the greater trochanter) reproduces the pain you usually feel during the day.
A 2025 systematic review of 212 piriformis syndrome cases found that 50.5 percent of diagnoses were made by symptoms, history, and physical examination alone, without imaging4. That tells you the clinical picture is usually distinctive enough to call without an MRI. If your symptoms fit the piriformis pattern, treat it as such while ruling out a disc through clinical follow-up only if symptoms do not respond.
Note that 38.2 percent of patients in that review had a history of blunt or indirect pelvic trauma (a fall on the buttock, a car accident, a sustained pelvic strain)4. If your piriformis pain showed up after a specific incident rather than gradually, the recovery timeline is usually longer and the case for a clinical evaluation is stronger.
Seated positions that aggravate vs relieve
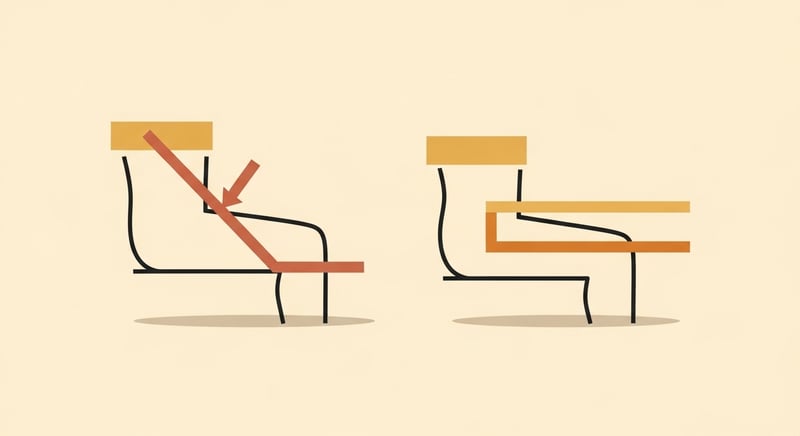
Two seated postures aggravate piriformis pain. The first is crossing the affected leg over the other knee in figure-four position. This stretches the piriformis statically and irritates an already-inflamed muscle. The second is sitting with the affected hip slightly externally rotated against a chair arm or wall. This compresses the piriformis against bone for the entire sitting duration.
The relieving postures share one principle: keep the affected hip in a neutral or slightly extended position, with the seat firm enough that the muscle is not getting pinned. A small lumbar wedge that tips the pelvis forward unloads the piriformis by extending the hip slightly. Sitting on a firm chair with the knees at or slightly above the level of the hips opens the hip-flexion angle in a useful direction.
For driving, a small wedge under the affected buttock to slightly raise it can take pressure off the muscle. For cycling, raising the saddle, switching to a wider saddle, and reducing standing-out-of-saddle riding all reduce piriformis load. For desk work, alternating between sitting and standing every 30 to 45 minutes is more useful than any specific seat configuration; a walking-style desk break every hour does the same job through movement.
A wallet, phone, or thick keychain in the back pocket of the affected side belongs in the avoid pile. The seat surface should be firm and flat. Soft couches and reclining chairs that drop the hips below the knees consistently provoke piriformis pain in symptomatic patients.
Stretching that actually works
The conventional piriformis stretch is the figure-four (lying on your back, ankle on opposite knee, pulling the knee toward your chest). It works, but a 2014 biomechanical study found that the standard position elongates the piriformis only about 12 percent2. The optimized position pulls more. With the hip in 115 degrees of flexion plus 40 degrees of external rotation plus 25 degrees of adduction, piriformis elongation increases to 30 to 40 percent. That is a meaningful difference for a stubborn muscle.
In practice this looks like a deeper figure-four with the knee pulled across the body more than the conventional version. Hold each side for 60 to 90 seconds. Repeat three times per session. Twice a day during a flare-up, once a day during recovery and maintenance.
A 2022 Cureus review found that pairing the stretch with sciatic nerve gliding (a separate exercise where you alternate flexing the hip and straightening the knee) reduces strain on the nerve more than tensioning techniques do3. The two together (stretch the muscle, glide the nerve) outperform either alone. The combined daily protocol takes about 10 minutes.
If you are someone who prefers strengthening over stretching for posture work, add hip-abductor and external-rotator strengthening (side planks, banded clamshells, single-leg bridges) on alternating days. The piriformis itself is an external rotator; if it is doing all the rotational work because the glute medius and glute max are weak, it stays under chronic load and never fully relaxes.
When to see a professional
Most piriformis syndrome resolves with positional changes and consistent stretching over four to eight weeks. The 2025 BMC Surgery systematic review found a 92.9 percent overall success rate combining conservative and surgical approaches, with conservative treatment alone succeeding in 41.1 percent of cases4. That means many cases need more than self-treatment, and a significant minority eventually need a procedure.
Three signals to escalate to a clinician. First, weakness in the leg or foot. Not pain, actual loss of strength when you try to push off or lift the toes. This suggests nerve compression has progressed beyond muscle irritation. Second, loss of bowel or bladder control. This is a red flag for cauda equina syndrome, a different and more serious spinal-emergency condition that needs immediate evaluation. Third, severe pain that does not respond to four to six weeks of consistent home treatment.
A physical therapist who specializes in hip and pelvic mechanics is the right next step in most cases. Imaging (MRI) is not usually needed for diagnosis but is sometimes used to rule out other causes when the clinical picture is unclear. Surgical release of the piriformis is uncommon and reserved for cases that fail extensive conservative treatment.
UpWise is an iOS app that scans your standing posture from a side photo and flags pelvic tilt and hip-rotation patterns. The app does not diagnose piriformis syndrome, but a baseline standing photo can show whether you stand in postural patterns that load the piriformis (anterior pelvic tilt with internal rotation of the affected leg), which gives you a starting point for the seated changes above. The daily routines also include the optimized 115-40-25 piriformis stretch and the sciatic-nerve glide pairing.
Frequently Asked Questions
Can piriformis syndrome go away on its own?
Often yes, with positional changes alone. Many mild cases resolve in two to four weeks once you stop the seated habits driving them, even without targeted stretching. Conservative treatment alone (positional change plus stretching) succeeds in about 41 percent of cases according to the 2025 systematic review. The cases that do not resolve in four to eight weeks usually need more focused work.
What sitting position is best for piriformis pain?
Knees at or slightly above the level of the hips, hip in a neutral or slightly extended position, no leg crossing on the affected side, no wallet in the back pocket, firm seat (not a soft couch). A small lumbar wedge that tips the pelvis forward helps. The single most consistent recommendation across the clinical literature is to break up sitting every 30 to 45 minutes.
How long does piriformis syndrome take to heal?
Most cases resolve in four to eight weeks of consistent positional changes plus daily stretching and nerve gliding. Cases triggered by trauma (a fall on the buttock, a pelvic strain) tend to take longer, sometimes three to six months. Cases that have been chronic for over a year before treatment have the lowest success rates with conservative care.
Is piriformis syndrome the same as sciatica?
Not exactly. Sciatica is a symptom (pain along the sciatic nerve distribution), and piriformis syndrome is one specific cause of that symptom. Most sciatica is caused by lumbar disc compression, not the piriformis. The two are distinguished by where the pain originates and what positions provoke it: piriformis pain worsens with sitting, while disc-driven sciatica often worsens with prolonged standing and bending forward.
Should I stretch through the pain?
Mild discomfort during the stretch is normal. Sharp shooting pain down the leg during the stretch means stop. The optimized 115-40-25 position should produce a strong stretch sensation in the buttock and outer hip, not a nerve-pain shoot down the leg. If the only stretch you can tolerate is conventional figure-four held briefly, start there and progress as the muscle calms down.