
Wrist Pain from Typing: A Posture-First Fix
Key Takeaways
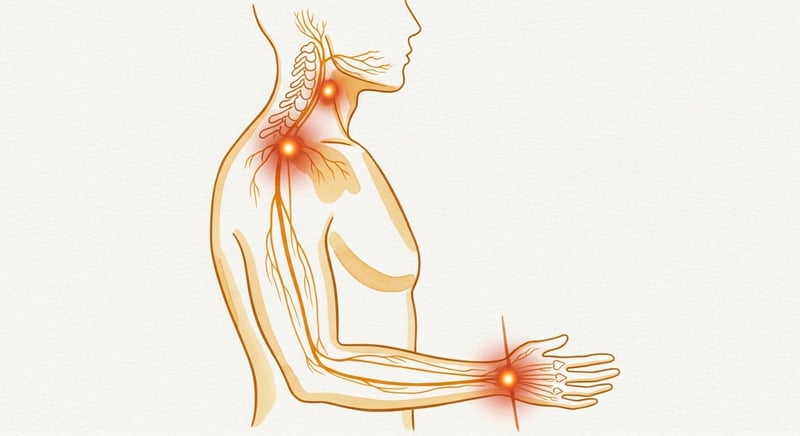
- Wrist pain from typing is usually a posture problem in disguise. The median nerve runs from the cervical spine through the shoulder and down the arm; compression upstream often shows up downstream as wrist pain.
- A 2009 JOSPT study found carpal tunnel patients had significantly more forward head posture and reduced cervical range of motion than healthy controls.
- A 2014 meta-analysis of nine worker cohorts found that prolonged exposure to non-neutral wrist posture roughly doubled the risk of carpal tunnel syndrome (pooled RR 2.01, 95% CI 1.65-2.43).
- Typing itself raises carpal tunnel pressure, and bending the wrist up (extension) or sideways (radial/ulnar deviation) raises it further.
- The fix is upstream first: chin tucks, scapular retraction, keyboard at elbow height, mouse close to the keyboard. Then targeted wrist flexor and extensor stretches.
Wrist pain from typing rarely starts at the wrist. The median nerve runs from your neck, through the shoulder, down the arm, and into the carpal tunnel, and pressure anywhere along that path can show up as wrist tingling and pain. A 2009 study in the Journal of Orthopaedic & Sports Physical Therapy found that carpal tunnel patients had significantly more forward head posture and less cervical mobility than healthy controls 1. The wrist position matters too: a meta-analysis of nine studies put the risk of carpal tunnel from prolonged non-neutral wrist posture at roughly double 2. This post covers why wrist pain is usually a posture problem, what neutral wrist position actually looks like, the cervical-and-scapular chain that drives it, the workstation fixes that work, and six stretches you can do today.
Why wrist pain is usually a posture problem
Most people with desk-job wrist pain assume the wrist itself is broken. It usually is not.
The median nerve, the main nerve that gets pinched in carpal tunnel syndrome, originates at the C5 through T1 cervical and upper-thoracic nerve roots. It travels down through the brachial plexus, under the pectoralis minor, through the antecubital fossa at the elbow, and finally through the carpal tunnel at the wrist. Compression at any point along that path produces symptoms that show up at and below the compression site.
The clinical name for this is double crush syndrome. A nerve already irritated upstream (say, by tight scalene muscles from forward head posture) is more vulnerable to irritation at a downstream site (the carpal tunnel). The two compressions do not add. They multiply. That is why the De-la-Llave-Rincón group at JOSPT found CTS patients had measurably more forward head posture and less cervical mobility than controls in both standing and sitting 1.
What this means in practice: if you only stretch the wrists, you may get partial relief. If you address the upstream chain, the same wrist symptoms often resolve without targeting the wrist at all. For the upstream end, see How to Fix Forward Head Posture, which covers the cervical mechanics, and How to Fix Rounded Shoulders, which covers the pectoralis minor and scalene chain that pinches the brachial plexus.
If you only stretch the wrists, you may get partial relief. If you address the upstream chain, the same wrist symptoms often resolve without targeting the wrist at all.
What neutral wrist position looks like, and what typing does
Neutral wrist position is straight. Your forearm, wrist, and hand form a single line, with the wrist neither bent up (extension) nor bent down (flexion) nor cocked sideways toward the thumb (radial deviation) or pinky (ulnar deviation).
In a 2008 study in the Journal of Orthopaedic Research, Rempel and colleagues measured carpal tunnel pressure during typing across different wrist positions. Three findings stood out. Wrist extension and flexion both raised pressure independently (p = 0.01). Radial and ulnar deviation also raised pressure (p = 0.03). And the activity of typing itself, separate from any held position, elevated pressure further (p = 0.001) 3. Static photos miss this third effect. Even at neutral, the act of pressing keys cycles pressure up and down inside the tunnel.
Now scale that up. The 2014 meta-analysis from You, Smith, and Rempel pooled nine studies of workers exposed to non-neutral wrist postures over time. The pooled relative risk for carpal tunnel was 2.01 (95% CI 1.65 to 2.43) 2. Roughly double. The signal got stronger with hours of exposure: more time at deviated angles, more risk.
If you watch your hands while typing now, three patterns are common. Wrists cocked up (extension) over a tall keyboard or against a thick laptop edge. Wrists deviated outward (toward the pinky) on a wide keyboard with hands held too close together. Wrists deviated inward (toward the thumb) on a narrow keyboard with shoulders held too wide. Each pattern compounds with hours and across years.
The cervical and scapular link
This is where most wrist-pain articles stop and just talk about the wrist. Here it gets more useful.
The De-la-Llave-Rincón paper measured the craniovertebral angle (a side-profile measurement of how far the head sits ahead of the shoulders) in patients with moderate carpal tunnel syndrome and matched controls. Patients had a significantly smaller angle (more forward head) and reduced cervical range of motion in every direction tested (p<.001) 1. The same paper found a positive correlation between forward head posture and cervical mobility loss across both groups, with r values between 0.27 and 0.45.
The mechanism is straight biomechanics. Forward head posture lengthens the scalenes on the front of the neck, which the brachial plexus passes through (specifically between the anterior and middle scalene). A taut scalene mildly compresses the nerve plexus at the source. Add rounded shoulders, which shorten the pectoralis minor that runs over the same plexus a few inches lower, and the nerve takes its second hit before it ever reaches the elbow. By the time it gets to the wrist, even normal typing pressure can push symptoms over threshold.
The implication for treatment: chin tucks and scapular retraction work on the wrists. They do not replace wrist mobility work, but they are often the missing piece. If your scapular position is the bigger driver, Where Your Shoulder Blades Should Sit, and How to Check covers what neutral looks like and three self-checks. UpWise's photo analysis flags both forward head posture and rounded-shoulder patterns from a single side-profile photo, which makes the upstream pattern visible without you having to guess.
Workstation setup that actually helps
Three changes do most of the work.
Keyboard at elbow height. Sit in your usual position with shoulders relaxed and elbows hanging by your sides. Bend your elbows to 90 degrees. Your hands should land on the keyboard at that height, with the wrists in a neutral straight line, not extended up to reach a keyboard that is too high. If your desk forces extension, lower the keyboard with a tray or raise the chair and use a footrest.
Mouse close to the keyboard. The mouse pushes the shoulder out into abduction the further it sits from the keyboard. That changes the whole arm angle, which forces the wrist into ulnar deviation (cocked toward the pinky) to keep the hand on the mouse. Use a smaller keyboard without a number pad if you can, and tuck the mouse against the right edge of the keyboard's main letter block.
Forearms supported, not the wrists. Resting the heels of your wrists on a desk edge while you type loads the carpal tunnel directly. Resting the forearms on the chair's armrests with the wrists hovering removes that contact load. A soft wrist rest can be useful at rest between bursts of typing, but typing on a wrist rest tends to keep the wrist extended.
For the deeper ergonomic picture (monitor, chair, keyboard tilt, sitting vs standing), see Keyboard and Mouse Ergonomics and The Complete Desk Posture Guide. UpWise's posture routine includes wrist mobility drills as part of the upper-body program, which works alongside an ergonomic setup rather than replacing it.
Six stretches that actually help
All six come from the Harvard Health and Cleveland Clinic protocols. Hold each for 15 to 30 seconds, four to five repetitions, two to three times a day 45.
Wrist flexor stretch. Extend one arm straight in front, palm up. Use the other hand to pull the fingers down and back gently until you feel a stretch along the underside of the forearm. Hold 20 seconds, switch sides.
Wrist extensor stretch. Extend one arm straight in front, palm down. Use the other hand to push the back of the hand down and toward the body until you feel a stretch on the top of the forearm. Hold 20 seconds, switch sides.
Prayer stretch. Press palms together in front of the chest, fingers pointing up. Slowly lower the hands toward the waist while keeping palms together, until you feel a stretch in both wrists. Hold 20 seconds. The Cleveland Clinic version recommends 3 to 5 repetitions 5.
Reverse prayer. Press the backs of the hands together in front of the chest, fingers pointing down. Slowly lift the hands toward the chin until you feel a stretch on the back of the wrists. Hold 20 seconds.
Median nerve glide. Hold one arm out straight, palm up, fingers pointed forward. Bend the wrist back so fingers point up. Now tilt the head away from that arm. You should feel a mild zinging stretch from neck to thumb. Hold 5 seconds, release, repeat 5 times. Targets the upstream-to-downstream nerve path directly.
Chin tucks. Sitting tall, slide your chin straight back (not down) so the back of the head moves toward the wall behind you. Hold 5 seconds, release. Ten reps. The chin tuck addresses the cervical end of the chain that the wrist stretches do not reach.
Run the first four daily, the last two as needed during desk breaks.
When to see a clinician
Most posture-driven wrist pain eases within 2 to 4 weeks of upstream and downstream work. A few patterns mean see a clinician sooner.
Numbness or tingling that wakes you up at night. The classic sign of more advanced carpal tunnel. The wrist often flexes during sleep, which compresses the tunnel further. A nerve conduction study can confirm.
Thumb-side hand weakness or visible thumb-base muscle wasting. Sustained median nerve compression eventually thins the thenar eminence (the muscle bulk at the base of the thumb). That is structural change, not just irritation. Get evaluated.
Symptoms that radiate up the arm to the shoulder, or come with neck pain plus arm numbness. The wrist may not be the primary problem. A cervical disc or nerve root issue can mimic CTS. Imaging and a clinical exam sort it out.
Pain not improving in 4 to 6 weeks of consistent work. The Cleveland Clinic guidance for wrist exercises is that pain should be at 3 or 4 or lower; any higher and it is time to see a healthcare provider 5. Persistent moderate pain past a month of changes is worth a hands-on look.
Frequently Asked Questions
Is my typing wrist pain definitely carpal tunnel?
Not necessarily. The classic signs of carpal tunnel are numbness or tingling in the thumb, index, middle, and half of the ring finger, often worse at night and easing when you shake the hand. Pain in the wrist itself without those nerve symptoms might be tendinosis, repetitive strain, or referred pain from upstream postural compression. A nerve conduction study from a clinician confirms or rules out CTS.
Should I wear a wrist brace while typing?
Wrist braces help short-term by holding the wrist in neutral overnight or during pain flares. Wearing them all day while typing tends to weaken the forearm muscles that should hold neutral on their own. Use a brace at night or during the worst few days, then taper off as upstream and stretch work takes over.
Does a vertical mouse help?
Often, yes. Vertical mice keep the forearm in mid-pronation (neutral handshake position) instead of fully pronated (palm-down) on a flat mouse. That removes one source of forearm and wrist tension. Most people who switch report less wrist strain within a week, though the bigger fix is usually keyboard and shoulder position.
Can ice or heat help typing wrist pain?
Ice helps acute inflammation, especially after a high-typing day or after stretching past tolerance. Heat helps chronic stiffness in the morning before stretching. Neither addresses the underlying posture or wrist position; they are symptom management, not a fix.
How long until stretches actually work?
Most people feel some change in 1 to 2 weeks of consistent work. Meaningful structural change in tissue extensibility takes 4 to 6 weeks. The cervical and scapular work tends to show fastest because the muscles up there are longer and respond quickly to stretch and strength load.