
Posture and Aging: How to Maintain Good Alignment After 50
Key Takeaways
- Posture decline after 50 is mostly muscle loss, not bone changes. That is the good news, because muscle is the part you can rebuild.
- A rounded upper back roughly doubles your fall risk because it pushes your weight forward, off the line your legs can catch.
- Back and shoulder strengthening works at any age. Most people see a straighter upper back within three months.
- Balance work and posture work are the same thing after 50. The muscles that hold you upright are the ones that stop a fall.
Posture changes as you age. Discs lose water content, vertebrae compress slightly, and muscles weaken if you do not use them. But the degree of change varies enormously between individuals, and most of the variation comes down to activity level, not genetics. People who stay physically active after 50 maintain better spinal alignment than sedentary people 20 years younger. The decline is not inevitable. It is conditional.
What Actually Changes in Your Spine After 50
Three things happen to your spine with age, and understanding which ones you can affect changes the entire conversation about aging posture.
First, disc dehydration. The intervertebral discs that cushion your vertebrae are about 80% water when you are young. By your 50s and 60s, they have lost a portion of that water content. Drier discs are thinner discs. This is why people get shorter as they age, losing about half an inch per decade after 40. The height loss is real, but it is small, and it does not, by itself, cause poor posture. It just means less cushioning between vertebrae.
Second, muscle loss. This is the big one. After 30, you lose roughly 3-5% of muscle mass per decade if you are not actively working to maintain it. By 50, that adds up. The erector spinae muscles that run along your spine, the core muscles that stabilize it from the front, the scapular muscles that hold your shoulders back: all of them weaken. Weak muscles cannot hold the spine in its neutral curves. The result is a gradual slumping, not because the bones have changed, but because the muscles have stopped doing their job. Understanding the science behind spinal alignment helps clarify why muscle strength matters more than most people realize.
Third, bone density changes. This one is structural and less modifiable, but it is also less common than you might think as a primary cause of poor posture. Osteoporosis-related vertebral fractures can cause permanent curvature changes, but they affect a fraction of older adults. Muscle loss affects everyone. That distinction matters because it means the most important intervention for age-related posture is exercise, not just calcium supplements.
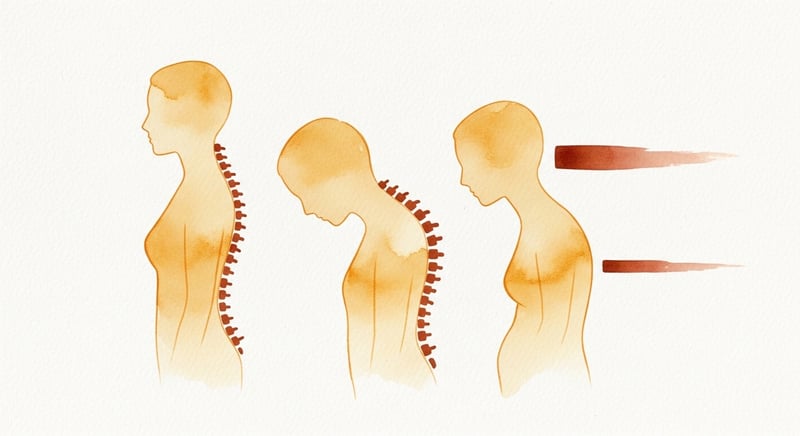
Kyphosis: The Forward Curve That Steals Your Balance
Kyphosis is the medical term for the forward curvature of the thoracic spine. Everyone has some degree of kyphosis. It is a normal part of spinal anatomy. The problem starts when it increases beyond the normal range, typically defined as a Cobb angle greater than 40 degrees. This condition, hyperkyphosis, affects 20-40% of adults over 60.1
The visible sign is the rounded upper back that people associate with old age. The functional consequence is more serious: your head shifts forward, your center of gravity moves ahead of your base of support, and your balance margin shrinks. Activities that require looking up (reaching a high shelf, checking traffic before crossing the street) become harder because your neck is already in a flexed position. For a detailed look at exercises that target this pattern, see our kyphosis exercise guide.
The good news from the research: much of age-related hyperkyphosis is postural, meaning it comes from muscle weakness and habitual positioning rather than structural bone changes. A 2009 study in the Journal of the American Geriatrics Society tested a spinal extension exercise program in adults over 60 with hyperkyphosis. After 12 weeks of targeted exercises (prone back extension, standing wall stretch, resistance band rows), the exercise group showed a measurable reduction in kyphosis angle compared to the control group.2 The participants were not young athletes. They were regular older adults with existing posture problems, and they improved.
The Bone Density Connection

Osteoporosis weakens bones by reducing mineral density. When it affects the thoracic vertebrae, those vertebrae can develop compression fractures, sometimes without any fall or obvious injury. The front of the vertebra collapses more than the back, creating a wedge shape. Stack several wedge-shaped vertebrae on top of each other and you get a permanent forward curve.
This is not the same as the postural kyphosis described above. Structural kyphosis from vertebral fractures cannot be fully reversed with exercise (the bone has physically changed shape). But the progression can be slowed, and the functional consequences can be managed. Weight-bearing exercise and resistance training both increase bone density and improve the muscle strength that compensates for structural changes.3
One important caution: if you have osteoporosis, avoid loaded spinal flexion. That means no heavy deadlifts, no sit-ups or crunches, and no bending forward to pick up heavy objects with a rounded back. These movements put maximum compressive force on the anterior (front) part of the vertebrae, exactly the area most vulnerable to fracture. Extension exercises (arching backward) and isometric core work (planks, bird-dogs) are safer alternatives.
Safe Exercises for Posture After 50
The exercises that help age-related posture are not dramatically different from the ones that help posture at any age. The difference is in the approach: lower intensity, more gradual progression, and extra attention to balance. The best posture exercises guide covers the full range, but here are the ones most relevant for adults over 50.
Thoracic extension over a foam roller. Lie face-up with a foam roller across your mid-back. Support your head with your hands. Gently arch backward over the roller. Hold for 15-20 seconds, then reposition the roller slightly higher or lower and repeat. This directly counteracts the thoracic rounding that accumulates from decades of sitting.
Wall angels. Stand with your back flat against a wall, arms up in a goalpost position with elbows and wrists touching the wall. Slowly slide your arms upward and back down, keeping contact with the wall throughout the movement. See our detailed wall angels guide for form tips. If you cannot keep your wrists against the wall, that tells you exactly how tight your chest and shoulder muscles have become. Start with 8-10 repetitions.
Seated resistance band rows. Sit on the floor or in a chair with a resistance band looped around your feet. Pull the band toward your chest, squeezing your shoulder blades together. This strengthens the rhomboids and middle trapezius, the muscles that pull your shoulders back and counteract the forward-rounded position. Two sets of 12-15 repetitions, three times per week.
Single-leg stands. Stand on one foot for 30 seconds. Hold onto a chair for support if needed. This is both a balance exercise and a posture exercise because it forces your core to stabilize against an asymmetric load. Switch sides. Work up to 60 seconds per side without support.
Balance, Falls, and the Posture Link
Falls are the leading cause of injury in adults over 65. And posture is directly connected to fall risk in a way that does not get enough attention.
When your thoracic spine rounds forward, your head moves ahead of your center of mass. Your body compensates by bending the knees slightly, shifting the hips backward, and shuffling the feet closer together. All of these compensations reduce your stability. A 2013 study in the journal Age and Ageing found that older adults with hyperkyphosis had 1.5 times the fall risk compared to those with normal thoracic curvature, and the risk increased with the severity of the curvature.4
This means that posture exercises for older adults are fall prevention exercises. They are the same thing. Strengthening the back extensors, improving thoracic mobility, and training balance all work together to keep the center of gravity over the feet where it belongs. The added benefit of UpWise posture tracking is that it gives you a visual measure of your alignment changes, so you can see if your thoracic curve is increasing before it becomes a balance problem.
Frequently Asked Questions
Is it too late to fix posture after 50?
No. While structural bone changes like vertebral wedging cannot be reversed, the muscular component of posture can improve at any age. Research on adults in their 60s and 70s shows measurable improvement in thoracic curvature after 12 weeks of targeted exercise. The changes take longer than they would at 30, but they do happen. Consistency matters more than intensity.
Does osteoporosis cause bad posture?
Osteoporosis can cause vertebral compression fractures, especially in the thoracic spine. These fractures cause individual vertebrae to collapse into a wedge shape, which increases the forward curvature of the upper back. This is the mechanism behind the "dowager's hump" you see in some older adults. But osteoporosis alone does not cause poor posture. The combination of bone loss and weak back muscles is what produces the visible change.
What exercises are safest for older adults with posture problems?
Gentle thoracic extension exercises (like lying face-down and slowly lifting the chest), wall angels, seated rows with a resistance band, and balance exercises like single-leg stands are all safe starting points. Avoid high-impact exercises and heavy overhead lifting. If you have osteoporosis, avoid loaded spinal flexion (bending forward with weight). Always start with lower intensity and progress gradually.
How does posture affect fall risk in older adults?
Increased thoracic kyphosis shifts your center of gravity forward, which reduces your balance margin. Studies show that older adults with hyperkyphosis have a 1.5 to 2 times greater risk of falls compared to those with normal curvature. The forward head position that accompanies kyphosis also affects your ability to see the ground ahead of you, compounding the risk.