
Dowager's Hump: What It Is, What It Isn't, How to Slow It
Key Takeaways
- Dowager's hump is the colloquial name for hyperkyphosis, an excessive forward curvature of the upper thoracic spine.
- Two versions exist: cosmetic posture hump (muscular, reversible) and clinical hyperkyphosis (structural vertebral wedging, slow to change).
- Hyperkyphosis affects roughly 20 to 40 percent of adults over 60, with women progressing faster than men due to post-menopausal bone loss.
- The 2017 SHEAF randomised controlled trial found that targeted spine-strengthening exercise reduced Cobb angle by 3 degrees over six months in older adults.
- Sudden mid-back pain, height loss greater than an inch in a year, or breathing difficulty needs a doctor, not a stretching routine.
The hump that appears at the base of the neck in older adults has a name, a cause, and two very different versions. Cosmetic posture hump is the soft-tissue rounding that comes from years of forward head and rounded shoulders. It shifts with stretching and strengthening. Clinical hyperkyphosis is structural, driven by vertebral wedging and bone loss, and changes much more slowly. Telling the two apart matters because the work that improves one barely touches the other.
What dowager's hump actually is
Dowager's hump is the colloquial name for excessive forward curvature of the upper thoracic spine and lower cervical region. The clinical term is hyperkyphosis. The StatPearls reference defines kyphosis itself as forward curvature of the spine in the sagittal plane, becoming hyperkyphotic when the angle measured by the Cobb method exceeds 40 degrees.1
How common is it? Excessive thoracic curvature shows up in roughly 20 to 40 percent of adults over 60.1 Women progress faster than men, partly because of post-menopausal bone density changes and partly because women's vertebrae are smaller to begin with.
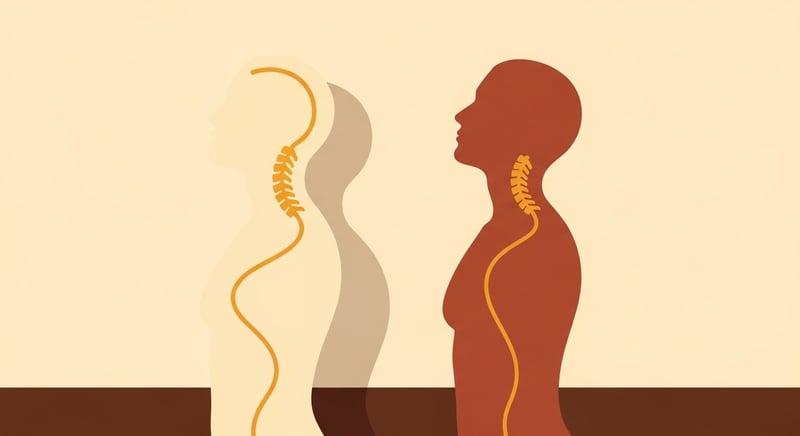
The visual sign is recognisable. The upper back rounds, the head juts forward, and a soft pad of tissue forms at the base of the neck. From the side, the chin sits ahead of the chest. The shape is not always painful in itself, but it carries a real load of secondary effects: restricted breathing capacity, balance changes, increased fall risk, and the daily strain of holding a heavier-than-designed forward load. The four natural curves of the spine are designed to balance loads. When the thoracic curve exaggerates beyond that design, the rest of the chain compensates.
Three groups develop it. Older adults, especially post-menopausal women, where bone density drives vertebral wedging. Long-term desk workers whose decades of forward-head posture create a muscular and fascial pattern that mimics structural kyphosis. Adolescents with Scheuermann's disease, a developmental form. This post focuses on the first two, since they are the most common reasons readers search.

The two types: cosmetic posture hump vs clinical hyperkyphosis
The crucial separation. Cosmetic posture hump and clinical hyperkyphosis are not the same condition.
Cosmetic posture hump (sometimes called postural kyphosis or the tech-neck hump) is what builds when forward head posture and rounded shoulders persist for years. The vertebrae themselves are still healthy. What you see on the outside is a combination: tight upper-trapezius and pectoralis muscles holding the shoulders forward, weak deep cervical flexors that fail to keep the head retracted, and over time, a fatty pad that develops at the cervicothoracic junction as the body deposits soft tissue around the chronically loaded area. The X-ray shows normal bone shapes. The spine is being held in a curved position by muscles, not by the bones themselves.
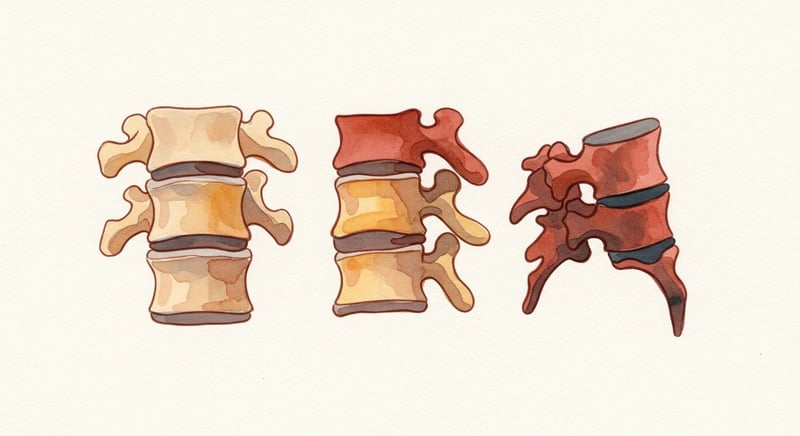
Clinical hyperkyphosis is structural. The vertebrae have changed shape, usually through a process called anterior wedging. The front edge of one or more thoracic vertebrae compresses faster than the back edge, so the bone itself becomes wedge-shaped instead of rectangular. Once a vertebra is wedged, it does not unwedge. The most common driver in older adults is osteoporosis. Low bone mineral density makes the vertebrae compress under everyday loads, often without a fall or an injury. A 2013 Sinaki study found that as thoracic curvature increases, regional bone density decreases. Pre-menopausal women with curvature exceeding 4 cm had nearly 4 times the risk of low bone mass.2
The simple test for which version you have. Take a side-profile photo standing relaxed, then a second standing tall and pulled back. If the hump shape softens significantly between the two photos, the dominant component is cosmetic. If it stays nearly identical, the structural component is leading. Most people over 50 with a visible hump have a mix of both, weighted increasingly toward structural as the years accumulate.
If the hump softens significantly between a relaxed photo and a stand-tall photo, the dominant component is cosmetic. If it stays identical, the structural component is leading.
How vertebral wedging actually happens
Wedging happens when bone is lost faster than it is rebuilt and when daily loads exceed what the weakened bone can tolerate. Three forces conspire.
First, hormonal. After menopause, estrogen drops sharply, and estrogen is one of the main signals that keeps bone-resorbing osteoclasts in check. The first five to seven post-menopausal years see the fastest bone loss, especially in the trabecular bone that makes up most of the vertebral body interior.
Second, mechanical. The thoracic spine is naturally curved forward. Gravity acts on the head and arms in a moment arm that loads the front of the vertebrae. Over thousands of small loading cycles, the front of the bone, which already faces higher compression than the back, compresses further. If bone density is normal, the bone remodels and holds. If density is low, micro-fractures accumulate.
Third, behavioural. Forward head posture roughly doubles the load on the lower cervical and upper thoracic vertebrae. A head that normally weighs 10 to 12 pounds applied straight down becomes the equivalent of 20-plus pounds when held forward. Multiply that by the seven to ten thousand hours per year a typical desk worker holds it that way, and the cumulative micro-load on already-weak bone is significant.
The clinical course is usually silent. Most vertebral compression fractures do not present with sharp acute pain. People notice height loss, a growing curve, or a partner saying you are getting shorter before they have any symptoms. By the time a fracture is visible on an X-ray, several smaller wedge fractures have often already happened. This is why the distinction between cosmetic hump and structural hyperkyphosis matters at the prevention stage. Posture work and strengthening can pause and partially reverse the cosmetic component. Once the bone has wedged, no amount of posture work straightens the actual vertebra. But the surrounding work still matters for balance, breathing, and whether further wedging happens.
What targeted exercise actually does (the SHEAF trial)
The strongest evidence available on whether targeted exercise can reduce existing hyperkyphosis comes from the Study of Hyperkyphosis, Exercise, and Function (SHEAF), a randomised controlled trial published in Osteoporosis International in 2017.3
The design: 99 community-dwelling older adults, mean age 70.6, with baseline kyphosis already at or above 40 degrees on Cobb-angle measurement. The intervention group received group spine-strengthening exercise and postural training, delivered by a physical therapist, one hour, three times per week, for six months. The control group attended four monthly health-education sessions over the same period, with no exercise.
The result: a 3.0-degree between-group reduction in Cobb angle, favouring the intervention. The authors note that the magnitude of this reduction approximates the change in Cobb angle from a single new vertebral fracture, but in the opposite direction. The exercise group also reported significantly improved self-image scores. Physical-function outcomes (gait speed, balance, sit-to-stand time) did not change measurably over six months in this population.
Three points readers should take from this. Six months of structured, three-times-weekly, physical-therapist-led work moved Cobb angle by 3 degrees. That is a real, measurable change, but it is not a transformation. People expecting to see the hump disappear in a season will be disappointed. Second, the change is meaningful precisely because it offsets the structural drift that would otherwise continue. Holding the line is the goal. Third, the program was specific. Targeted spine-strengthening and postural work, not generic exercise. General gym training does not reliably move kyphosis in this population.
The lesson. In clinical hyperkyphosis, the right exercise pattern can reverse some of the curve and, more importantly, slow the progression that drives further wedging. In cosmetic posture hump, the same kinds of exercises move the visual outcome much faster because there is no structural ceiling on what the muscles can change.
A daily protocol, and when to see a clinician
For both versions of the hump, the daily protocol overlaps. Stretch what is short. Pectoralis minor and major are usually tight in long-term forward-head posture. The doorway chest stretch held three times daily for 30 seconds each begins to release the front of the chest. The thoracic spine mobility work opens the stiff segments of the upper spine that rotate poorly in the rounded position.
Strengthen what is weak. Deep cervical flexors fail first. The chin-tuck, performed lying on the back with a small towel under the head, retrains the muscle pattern that holds the head retracted. Mid-trapezius and rhomboids hold the shoulder blades back. Prone Y-T-W lifts and band pull-aparts target them directly. The full posture-exercise progression sits in the comprehensive exercise guide.
Load the spine, carefully. The SHEAF trial used spine extensors as the primary strengthening focus. Prone back-extension work, scaled to tolerance, is the main lever. Add resistance gradually. People with diagnosed osteoporosis or a history of compression fractures should consult a physical therapist before starting loaded extension work. Too much extension under load can cause exactly the kind of fracture you are trying to prevent.
Move daily. Six minutes of integrated mobility and strengthening every morning beats one ninety-minute session per week. The SHEAF protocol used three weekly hours, and that level of dose is what produced the 3-degree shift over six months. At home, daily ten-to-fifteen-minute sessions are the realistic target.
When to see a clinician. Any of the following warrants a doctor's visit, not a stretching routine. Sudden new mid-back pain, especially after a minor fall or even no fall, can indicate a vertebral compression fracture. Loss of more than one inch of height over a year. Difficulty taking a full breath. Numbness, tingling, or weakness in the arms or legs. Any combination with a history of osteoporosis, long-term steroid use, or prior vertebral fracture. The earlier a structural change is detected, the more options exist for slowing it.
UpWise is an iOS app that scores spine alignment from a single side-profile photo and prescribes the specific cervical and thoracic exercises that target the hump-driving muscle pattern. It does not diagnose hyperkyphosis but flags the posture pattern and tracks how the alignment scores change over weeks. For older readers concerned about their parents' posture, the same single-photo workflow runs on any iPhone.
Frequently Asked Questions
Can a dowager's hump be fully reversed?
It depends on the version. Cosmetic posture hump driven by muscle imbalance and soft-tissue accumulation can soften substantially with consistent work over months. Clinical hyperkyphosis driven by vertebral wedging cannot be fully reversed because once a vertebra has wedged, the bone shape does not return. The SHEAF trial showed that targeted exercise can reduce Cobb angle by about 3 degrees over six months in older adults with established hyperkyphosis. That is a real change but not a transformation.
How do I know if my hump is muscular or structural?
Take two side-profile photos: one standing relaxed, one standing tall and consciously pulled back. If the hump shape softens significantly between the two photos, the dominant component is muscular. If it stays nearly identical, structural change is leading. Most people over 50 with a visible hump have a mix of both. A DEXA bone density scan and a thoracic spine X-ray confirm the structural component if your doctor suspects it.
Are posture braces useful for dowager's hump?
For cosmetic posture hump, braces provide short-term cueing but do not strengthen the muscles that need to hold the position long-term. For clinical hyperkyphosis, kyphosis-specific braces (different from generic posture correctors) are sometimes prescribed by clinicians to offload painful vertebral fractures during healing. They are a clinical tool, not a self-prescribed device. Exercise therapy has stronger evidence for both versions.
Does swimming help reduce a hump?
Swimming, particularly backstroke, can help by strengthening the upper-back extensors and opening the front of the chest. It is gentler on bone-loaded joints than ground exercises, which makes it suitable for older adults who cannot tolerate floor work. It does not replace targeted spine-strengthening work but is a strong complement, especially for people who already enjoy the pool.