Posture During Pregnancy: Safe Alignment Tips by Trimester
Key Takeaways
- Your joints start loosening in the first trimester, well before your belly shows, so back support matters from day one.
- Most pregnant women get back pain, and it usually peaks in the third trimester as your spine curves to balance the bump.
- Cat-cow, pelvic tilts, and wall squats are safe the whole way through and target the exact muscles each stage stresses.
- Sleep on your side with a pillow between your knees once you are past the first trimester.
- The strength you build now is what helps you recover faster after the baby arrives.
Pregnancy changes your posture whether you pay attention to it or not. Hormones loosen your ligaments, your growing belly pulls your spine forward, and your center of gravity shifts by several inches over nine months. These changes are normal and necessary. They are also the reason 50-70% of pregnant women develop back pain. Trimester-specific posture adjustments can reduce that pain and set you up for a smoother recovery after delivery.
We wrote this guide because pregnancy posture advice tends to fall into two camps. One camp says "stand up straight" and leaves it at that. The other overwhelms you with 30 exercises and no context for when to do them. The reality is that what your body needs in week 10 is different from week 30. Your alignment changes, your balance shifts, and the exercises that help need to change with them.
Why Pregnancy Changes Your Posture
Two forces reshape your spine during pregnancy. One is mechanical: a growing weight in your abdomen pulls your pelvis forward and your lumbar spine into a deeper curve. The other is hormonal, and it starts earlier than most people expect.
Relaxin is a peptide hormone that your body produces starting in the first trimester. Its primary job is to loosen the ligaments around your pelvis so the birth canal can widen during delivery. But relaxin does not target the pelvis exclusively. It circulates through your entire body, affecting ligaments in your spine, knees, ankles, and feet. A 2004 study in the Annals of the Rheumatic Diseases found that joint laxity increases throughout pregnancy and peaks in the third trimester, with the sacroiliac joint showing the most dramatic increase in mobility.1
What this means practically: the ligaments that normally hold your vertebrae in alignment become stretchier. Your spine depends more on muscle strength to stay stable, at the same time that your muscles are dealing with a shifting load. That is why pregnant women who were physically active before pregnancy tend to have less back pain. Their muscles were strong enough to compensate for the ligament laxity.
The postural changes are not random. They follow a predictable pattern across the three trimesters, and understanding that pattern is the key to managing them. Research published in the European Spine Journal tracked 105 pregnant women from weeks 12 through 36 and found that lumbar lordosis increased by an average of 7 degrees, with the steepest increase between weeks 20 and 32.2 That maps directly to the period of fastest fetal growth.
First Trimester: The Invisible Shift
Your belly is not showing yet. You might not even have told anyone about the pregnancy. But inside, relaxin is already circulating and your ligaments are beginning to loosen. Most women do not notice posture changes during the first trimester because the mechanical load has not shifted yet. The belly is too small to affect your center of gravity.
The first trimester is the best time to build the habits and strength that will protect you later. Think of it as pre-loading your body for the changes ahead.
What to focus on: core awareness. Not crunches or planks on the floor (those become inappropriate as the belly grows), but exercises that teach you to engage your deep core stabilizers, the transverse abdominis and pelvic floor muscles. These are the muscles that support your spine from the inside. Strengthening them now gives you a foundation that persists through the second and third trimesters even as relaxin loosens everything else. If you have not worked on your posture habits before, our daily posture habits guide covers the foundational patterns that apply here.
Watch for: fatigue-related slouching. First-trimester exhaustion is real, and when you are bone-tired, your posture collapses. Rather than fighting it with willpower, use environmental cues. Put a small cushion behind your lower back when you sit. Set a phone timer to stand up every 45 minutes. These external reminders do the work so you do not have to remember.

Second Trimester: Center of Gravity Moves
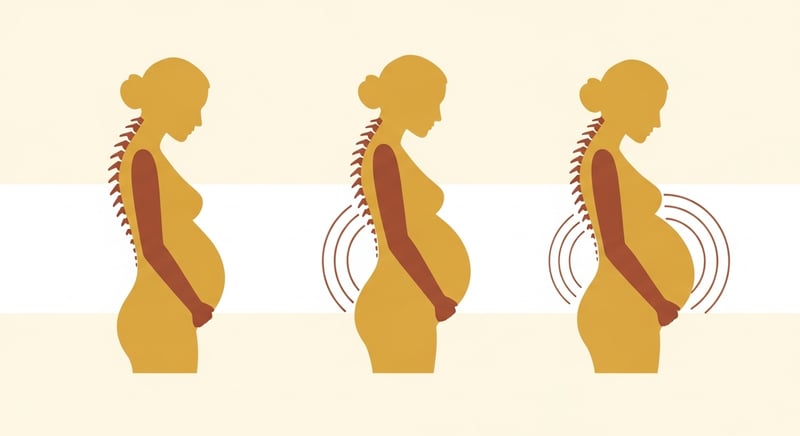
Weeks 14 through 27 are when most women first notice their posture changing. The belly is growing visibly, the uterus has risen above the pelvis, and your weight distribution is shifting forward. You might catch yourself swaying backward when you stand still. That backward lean is your body's instinct to keep from tipping forward. It works for balance, but it hammers your lower back.
"The backward lean that feels natural during pregnancy is your body choosing balance over back health. Every degree of extra lordosis adds compressive load to the lumbar discs."
The second trimester is when targeted posture exercises start to matter most. The goal is not to fight the postural shift (you cannot, and should not, stop your belly from growing), but to manage the compensation patterns that cause pain. The primary compensation is excessive lumbar lordosis. The secondary one is thoracic kyphosis: your upper back rounds forward because the weight in front is pulling your shoulders down.
A study in the Journal of Bodywork and Movement Therapies found that pregnant women who participated in a structured exercise program during the second trimester had 40% lower pain scores by the third trimester compared to a control group.3 The exercises were not complicated. Cat-cow stretches, standing pelvic tilts, and modified squats, all done for 20 minutes, three times per week.
One change specific to the second trimester: your rib cage expands. The growing uterus pushes your diaphragm upward, and your lower ribs flare outward to accommodate. This changes your breathing mechanics and can contribute to thoracic stiffness. Gentle thoracic rotation stretches (seated twists with support) help maintain mobility in the mid-back.
Third Trimester: Maximum Compensation
Weeks 28 through 40 are the peak of postural change. Your baby is gaining roughly half a pound per week, your belly is at its largest, and relaxin levels are at their highest. The lumbar curve is at maximum lordosis. Your pelvis has tilted forward. Your thoracic spine has rounded to counterbalance. And your feet may have flattened slightly from the combination of weight gain and ligament laxity.
Back pain peaks during the third trimester. A systematic review in BMC Pregnancy and Childbirth analyzed 28 studies and reported that the prevalence of low back pain during pregnancy ranged from 25% to 90%, with the highest rates in the third trimester.4 The range is wide because studies measured pain differently, but the trend is consistent: it gets worse as the belly gets bigger.
By the third trimester, your exercise options are more limited. Lying on your back is out (the weight of the uterus compresses the vena cava, the large vein that returns blood to your heart). High-impact anything is out. But the exercises you can still do, standing pelvic tilts, supported wall squats, seated cat-cow, and hip circles on a birth ball, are the ones that matter most for lower back pain relief.
"In the third trimester, exercise is not about fitness. It is about pain management, circulation, and preparing your pelvic floor for delivery."
Walking remains one of the best things you can do. It is low impact, it maintains circulation in your legs (reducing swelling), and the upright position encourages better spinal alignment than sitting. Keep walks moderate: 15-30 minutes at a comfortable pace. If you feel pelvic pressure or heaviness, that is your signal to stop and rest.
Watch for warning signs during the third trimester. Numbness or tingling down one or both legs could mean the baby's position is compressing the sciatic nerve. Rhythmic back pain that comes in waves could be contractions. Sharp, sudden pain after a fall needs immediate medical attention. Most pregnancy back pain is muscular and manageable, but these symptoms need a doctor's evaluation.
Safe Posture Exercises by Trimester
These exercises are grouped by when they are most useful, but most of them are safe throughout all three trimesters unless noted. Always check with your OB-GYN or midwife before starting a new exercise routine. Stop any exercise that causes pain, dizziness, or shortness of breath.
All trimesters: Cat-cow stretch. On hands and knees, alternate between arching your back (cow) and rounding it (cat). This mobilizes the entire spine, relieves lumbar compression, and strengthens the deep core muscles. Do 10-15 repetitions, twice daily. In the third trimester, widen your knees to make room for your belly. The core strengthening guide covers this exercise in more detail.
All trimesters: Standing pelvic tilts. Stand with your back against a wall. Gently flatten your lower back against the wall by tucking your pelvis under. Hold for 5 seconds, release. Repeat 10 times. This directly counteracts the excessive lordosis that causes most pregnancy back pain.
First and second trimester: Modified bird-dog. On hands and knees, extend one arm forward and the opposite leg backward. Hold for 5 seconds. This trains the stabilizing muscles on both sides of your spine. In the third trimester, keep both knees on the ground and just extend the arm.
Second and third trimester: Birth ball circles. Sit on a stability ball (65cm or 75cm depending on your height) and make slow circles with your hips. This opens the pelvis, maintains hip mobility, and gently works the pelvic floor muscles. Start with 10 circles in each direction.
Third trimester: Supported wall squat. Lean against a wall with your feet shoulder-width apart and about 18 inches forward. Lower into a quarter squat (not deep) and hold for 10-15 seconds. This strengthens your glutes and quadriceps, which support your pelvis and reduce the load on your lower back.
Sleeping Positions and Pillow Support

Sleep is where posture gets tricky during pregnancy. You spend 7-9 hours in one position, and the wrong position can undo the work you put in during the day.
After the first trimester, side sleeping is the standard recommendation. Left side is slightly preferred because it keeps the uterus off the inferior vena cava and improves blood flow to the placenta. But both sides are fine. Do not stress if you wake up on your right side. A study in Obstetrics and Gynecology found that the left-versus-right distinction matters most in the final weeks of pregnancy and that both side positions are safer than supine.5
The pillow between the knees is not optional comfort. It keeps your hips level. Without it, the top leg drops forward, rotating your pelvis and putting a twisting force on your lower back. A regular bed pillow works, but a body-length pregnancy pillow is more convenient because it stays in place when you shift positions. For more on how sleep position affects your spine, see our sleeping posture guide.
One more pillow tip: a small, thin pillow under your belly. As the belly grows, side sleeping without belly support lets gravity pull your abdomen downward, which rotates your spine. A folded towel or thin pillow underneath provides just enough lift to keep your spine in neutral alignment. Many women discover this on their own through trial and error, but knowing about it early saves a lot of uncomfortable nights.
When to Use a Maternity Support Belt
Support belts are controversial in the posture world. The general advice is that external support weakens the muscles it replaces. That is true for standard posture braces worn all day. Maternity belts are a different situation because the load they are supporting (a growing baby) is temporary and increasing beyond what even strong core muscles can comfortably handle.
A 2015 review in the Journal of Clinical Nursing found that maternity support belts reduced pain intensity during activities like walking and prolonged standing, though they did not eliminate pain entirely.6 The benefit was most pronounced in the third trimester and in women with physically demanding jobs.
"Use a maternity belt like you would a back brace after surgery: during high-load activities, not as a permanent crutch. Your muscles still need work."
When a support belt makes sense: standing for more than 30 minutes at a stretch, long walks during the third trimester, grocery shopping or carrying a toddler, and jobs that require prolonged standing or walking. When to skip it: sitting at a desk (your chair provides the support), lying down, and during exercise (it restricts movement). Continue your posture exercises whether you wear a belt or not. The belt manages pain in the moment. The exercises build the strength you need for postpartum recovery.
Building the Bridge to Postpartum Recovery
Pregnancy posture work is not just about the nine months of pregnancy. The muscle strength and body awareness you develop now directly affect your recovery after delivery. Relaxin levels do not drop to pre-pregnancy levels until several months postpartum. Your ligaments remain loose. And now you are lifting, carrying, and nursing a baby, all activities that demand good posture from a body that has spent nine months adapting to a different load pattern.
Women who maintained posture exercises during pregnancy report faster return to pre-pregnancy alignment, less postpartum back pain, and fewer issues with diastasis recti (the separation of the abdominal muscles that occurs during pregnancy). The transverse abdominis work you did in the first trimester pays dividends here. That deep core muscle is the primary one that closes the abdominal gap after delivery.
After delivery, your immediate priorities shift from managing a forward load to recovering from the birth itself. But within the first few weeks, gentle pelvic floor contractions and transverse abdominis engagement can resume. By 6-8 weeks postpartum (with your doctor's clearance), you can return to the full set of posture exercises. The women who do this consistently report better outcomes than those who wait until postpartum pain forces them to act. UpWise can help track your alignment progress through this transition and suggest exercises appropriate for your recovery stage.
Frequently Asked Questions
Is it safe to do posture exercises during pregnancy?
Yes, with modifications. Exercises like cat-cow stretches, pelvic tilts, and supported wall squats are generally safe throughout pregnancy. Avoid lying flat on your back after 20 weeks, and stop any exercise that causes pain, dizziness, or shortness of breath. Always check with your OB-GYN or midwife before starting a new exercise routine during pregnancy.
Why does my lower back hurt so much during pregnancy?
Two factors collide. First, relaxin hormone loosens your pelvic joints and spinal ligaments, reducing the stability your lower back normally relies on. Second, as your belly grows, your center of gravity shifts forward, pulling your lumbar spine into a deeper curve (lordosis). The muscles in your lower back work harder to compensate, and they fatigue. This combination is why 50-70% of pregnant women report low back pain, most commonly in the second and third trimesters.
Should I wear a maternity support belt for posture?
A maternity support belt can help during the third trimester by lifting some of the belly weight off your pelvis and lower back. Research shows these belts reduce pain intensity in the short term. But they are not a substitute for muscle strengthening. Use a support belt for high-activity periods (long walks, standing at work) and continue doing posture exercises to maintain the muscle strength you will need postpartum.
What sleeping position is best for posture during pregnancy?
Side sleeping, preferably on your left side, is recommended after the first trimester. Place a pillow between your knees to keep your hips aligned and reduce strain on your lower back. A small pillow under your belly provides additional support. Avoid sleeping flat on your back after 20 weeks, as the weight of the uterus can compress the vena cava and reduce blood flow.
When should I see a doctor about pregnancy-related back pain?
See your healthcare provider if your back pain is severe enough to limit daily activities, if it comes with numbness or tingling down your legs (which could indicate nerve compression), if the pain is rhythmic and comes in waves (which could be preterm contractions), or if it started after a fall or injury. Most pregnancy back pain is muscular and manageable with posture adjustments and exercise, but these red flags need medical evaluation.