
SI Joint Pain and Posture: What Aggravates It and What Helps
Key Takeaways
- The sacroiliac joint sits between the sacrum at the bottom of the spine and the ilium of the pelvis, transferring upper-body weight to the legs. Total motion is only 2-4mm in any direction.
- SI joint dysfunction accounts for an estimated 15-30% of low back pain cases, with StatPearls putting the upper end at 25%.
- Pain typically presents in the lower back, buttock, or back of the thigh on one side, and gets worse after sustained sitting, standing in one position, or hip rotation.
- Anterior pelvic tilt and asymmetric sitting (legs crossed always to one side, wallet in one back pocket, leaning into one armrest) are the main postural drivers.
- Lumbopelvic stabilization training has been shown to reduce disability scores by about 50% in research; non-specific exercise does not produce the same effect.
SI joint pain hides in plain sight. People feel it in the lower back, the buttock, sometimes down the back of the thigh, and they call it back pain. The sacroiliac joint is the small but heavily-loaded link between the sacrum at the bottom of the spine and the ilium of the pelvis, and one literature review estimates it accounts for 15 to 30 percent of low back pain cases 2. Posture matters here more than in most pain syndromes because the SI joint is built for stability and barely moves at all. Anything that loads it asymmetrically, from a slouched chair to a leg-length difference to an anteriorly tilted pelvis, will eventually inflame it. This post covers what the joint does, where the pain shows up, the postures that aggravate it, three self-checks, and the exercises that actually help.
What the SI joint actually does
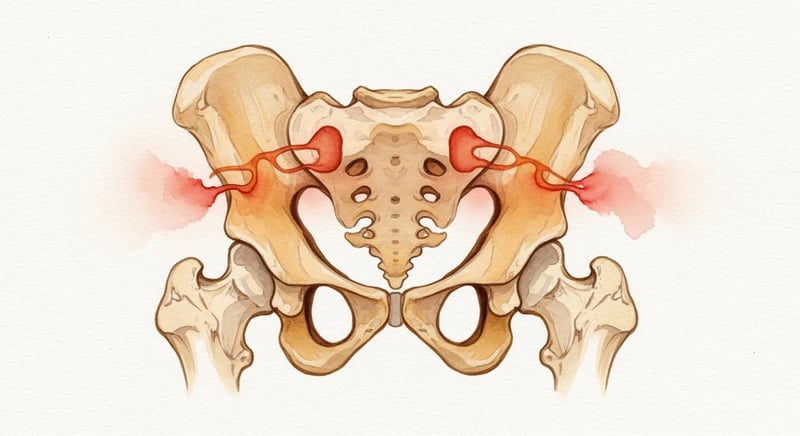
The sacroiliac joint sits at the back of the pelvis where the sacrum (the wedge-shaped bone at the base of the spine) meets the ilium (the upper, flared part of the hip bone). You have one on each side, just below the dimples of the lower back. Anatomically, the joint is part synovial in the front and part fibrous ligament in the back. That hybrid structure is unusual.
The joint's job is weight transfer. Upper-body load comes down through the lumbar spine, hits the sacrum, and gets dispersed into the two ilia and out into the legs. Total motion across the joint is roughly 2 to 4 millimeters in any direction 1. It is built to hold position, not move. Strong sacroiliac ligaments and the surrounding glute, multifidus, and transverse abdominis muscles keep the joint locked in.
That stability is also why dysfunction matters. When the surrounding system fails to stabilize the joint, every step transmits a small shear across an inflamed surface. Walking can hurt. Sitting can hurt. Rolling over in bed can hurt. The joint itself has a dense supply of pain nerves, and a 2000 study mapped 18 distinct pain referral patterns coming off it: posterior or lateral thigh pain in about half the cases, pain past the knee in 28%, even foot pain in 14% 1. For the broader picture of how lumbopelvic alignment ties into spinal posture, see Spinal Curves: What the Four Natural Bends in Your Back Do.
How common is it actually
SI joint pain is far more common than most people are told.
Barros and colleagues, reviewing the SI joint pain literature in Federal Practitioner in 2019, put the prevalence of SI joint dysfunction at 15 to 30 percent of low back pain cases 2. The StatPearls entry on Sacroiliac Joint Pain places the upper end of that range at 25 percent 1. Either way, somewhere between one in seven and one in three people who think they have generic low back pain are actually dealing with the SI joint specifically.
The under-diagnosis is partly the joint's fault. SI pain mimics lumbar pain, sciatica, and hip pain. There is no single physical test that nails the diagnosis on its own, which is why physical therapists run pain provocation tests in clusters and call it positive when 3 of 5 reproduce the pain 5. Without that pattern the pain often gets routed to a different label and treated as something else for months.
Risk factors that push you toward the SI side of the diagnosis: a history of lumbar fusion (the load above has to go somewhere), scoliosis, an actual leg-length difference, pregnancy, sustained athletic activity that loads the pelvis asymmetrically, or a chronic gait abnormality from an old injury 2.
Somewhere between one in seven and one in three people who think they have generic low back pain are actually dealing with the SI joint specifically.
How posture makes it worse
Two postural patterns drive most SI joint dysfunction.
The first is anterior pelvic tilt, the same pattern that drags the lumbar curve into hyperlordosis. When the pelvis tips forward at the hip, the sacrum rotates with it and the SI joint loads asymmetrically. Hold that position for hours of sitting and the surrounding ligaments stretch out. For more on the underlying tilt pattern, see Anterior Pelvic Tilt: What It Is and How to Fix It.
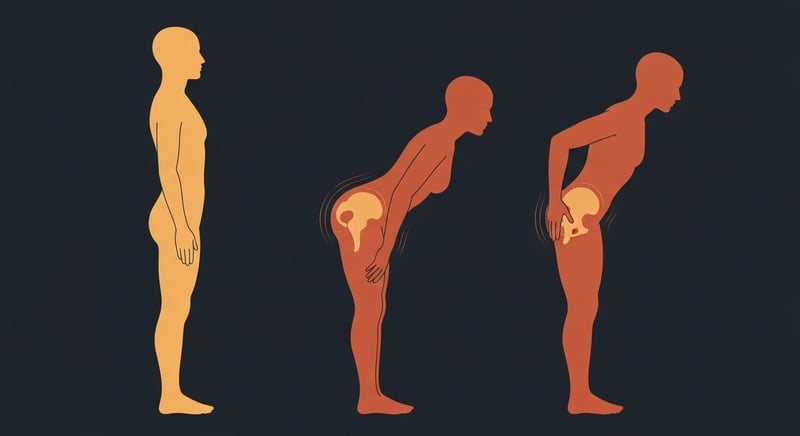
The second is asymmetric sitting. Crossing the legs always to the same side. Carrying a wallet in one back pocket. Leaning into one armrest. Sitting on a soft couch that lets one hip sag. All four put a constant rotational shear across the SI joint on one side. Cleveland Clinic notes SI joint pain typically gets worse after sitting or standing in one position for a long time, and worsens with hip rotation 4.
Long sitting itself is hard on the joint even with good symmetry. The glute and multifidus complex that locks the joint in place switches off when you sit. The erector spinae take over but cannot replace the deeper stabilizers, and after a while everything fatigues onto the joint surface. Hip Pain From Sitting covers the broader sitting-load problem.
UpWise's photo analysis catches anterior pelvic tilt and pelvic asymmetry from a single side-profile photo, surfacing these patterns before you have to guess from how things feel.
Three self-checks to localize the pain
Most people who think they have low back pain cannot tell whether the joint actually involved is the lumbar spine, the SI joint, or the hip. Three quick checks help.
The Fortin finger test. Point with one finger to the most painful spot on your back. If the finger lands within an inch of the small dimple just lateral and slightly below the lumbar spine on one side (the posterior superior iliac spine), the SI joint is the most likely source. SI pain is usually one-sided, dull or sharp depending on the day, and very localizable.
The FABER (Patrick) test. Lie face up. Bend one knee and place that ankle on the opposite knee, so the bent leg makes a figure-4. Let the bent knee drop toward the floor. Pain in the back of the pelvis on the same side as the bent leg suggests SI joint involvement. Pain in the front of the hip or groin instead suggests hip pathology. The FABER test is one of the more specific provocation maneuvers for SI joint dysfunction, especially when combined with the thigh-thrust and distraction tests 5.
The standing-up test. SI joint pain has a distinctive pattern: it often eases when you walk for a few minutes and worsens when you stand up from sitting. Try this. Sit for 20 minutes. Stand up slowly. If the first 30 seconds of standing produce a sharp pull at the back of the pelvis on one side and walking eases it, the SI joint is the most likely culprit.
None of these are diagnostic. They are filters. SI joint pain is officially diagnosed by clinical clusters of provocation tests or a fluoroscopy-guided injection 2. The home checks tell you whether to ask a clinician to look at the SI joint specifically.

Four exercises that stabilize the joint
The exercise principle for SI joint pain is specific over general. Laslett's evidence review put it bluntly: lumbopelvic stabilization training reduced disability scores by about 50%, while exercises not specifically targeting lumbopelvic stability were no more effective than other treatments 5. Al-subahi's systematic review echoed it: manipulation and targeted exercise both work, non-specific exercise underperforms 3.
Four drills target the right muscles.
Glute bridge. Lie face up, knees bent, feet flat. Press through the heels and lift the hips until knees, hips, and shoulders form a straight line. Squeeze the glutes hard at the top. Hold 3 seconds, lower. Two sets of ten. The glutes are the prime stabilizers of the SI joint.
Clamshell. On your side, knees stacked and bent at 90 degrees, feet together. Lift the top knee like a clamshell opening, hold 2 seconds, lower. Fifteen each side. Targets the gluteus medius, the side-stabilizer controlling one-leg load.
Bird-dog. On hands and knees, extend the opposite arm and leg parallel to the floor. Hold 5 seconds, return, switch. Ten each. Engages the deep multifidus and obliques across the SI region without compressive load.
Dead bug. Lie face up, arms straight up, legs in tabletop. Slowly lower the opposite arm and leg toward the floor without arching the lower back, return, switch. Ten each. Trains lumbopelvic control under controlled load.
Run these once a day. UpWise builds a routine around the patterns it picks up from your photo. For the broader strengthening picture, see Core Strengthening for Posture.

When to see a clinician
Most postural SI joint pain calms within a few weeks of consistent stabilization work and removing the postural drivers. A few patterns mean see a clinician sooner.
Pain that radiates past the knee with numbness or tingling in the foot. Could be SI referral but could also be sciatica or a lumbar disc problem. The two need different treatments.
Bilateral SI pain, morning stiffness lasting more than 30 minutes, age under 45 at first onset. That cluster raises suspicion for an inflammatory spondyloarthropathy, treated very differently from mechanical SI pain.
Pregnancy or postpartum SI pain. Hormonal ligament laxity makes the joint more mobile and easier to inflame. Common, treatable, but benefits from a clinician who knows pelvic-floor mechanics.
Pain that does not improve in about a week. Cleveland Clinic's standard is straightforward: if it does not start getting better on its own in roughly a week, it is worth getting eyes on it 4. For how to distinguish SI from lumbar discogenic pain, Lower Back Pain and Posture has more detail.
Frequently Asked Questions
Where does SI joint pain hurt exactly?
SI joint pain typically localizes to the lower back, the buttock, or sometimes the back of the thigh on one side. Pain usually sits within an inch or two of the small dimple in the low back (the posterior superior iliac spine) and can radiate down past the knee in about 28% of cases 1. The hallmark is one-sidedness; pain that is perfectly symmetric across the spine is more often lumbar than SI.
Can sitting cause SI joint pain?
Yes, especially asymmetric or prolonged sitting. Crossing the legs always to the same side, sitting on a wallet, leaning into one armrest, or sustained sitting in any position all load the SI joint asymmetrically. Cleveland Clinic notes SI joint pain typically gets worse after sitting or standing in one position for a long time 4.
How is SI joint pain different from sciatica?
Both can refer pain down the leg, which is why they get confused. Sciatica is nerve-root pain that follows the sciatic nerve distribution (down the back of the thigh, calf, sometimes the foot) and is usually caused by lumbar disc compression. SI joint pain is joint pain that can refer in similar regions but does not follow a clean nerve dermatome and is reproduced by SI provocation tests like FABER. A clinician's diagnostic cluster sorts them apart.
Should I rest or move with SI joint pain?
Move, but specifically. Bed rest tends to make SI pain worse because the stabilizing glutes and multifidus deactivate further. Targeted lumbopelvic stabilization (glute bridges, clamshells, bird-dog) is the highest-yield work 5. Avoid aggravating positions during the acute phase: deep crossed-leg sitting, asymmetric standing, twisting under load. Walking is usually fine and often helpful.
How long does SI joint pain take to heal?
Acute postural SI joint pain often eases within 1 to 4 weeks of consistent stabilization work and removing postural drivers 3. Pain that lingers beyond a month, gets worse, or comes with neurological symptoms warrants imaging and a clinician's diagnostic cluster. Pregnancy-related SI pain has its own timeline and usually improves postpartum once ligament laxity normalizes.