
Posture for Fall Prevention in Older Adults: The Mechanics and the 12-Week Protocol
Key Takeaways
- More than 1 in 4 adults aged 65 and older fall each year. Falls drive about 3 million ED visits, 1 million hospitalizations, and 43,000 deaths annually in the US, and the numbers are rising.1
- Three posture mechanics carry the largest modifiable share of fall risk: a forward-rounded thoracic spine (hyperkyphosis), stiff ankles with weak toe strength, and weak hip abductors plus glutes.
- Hyperkyphosis is prospectively associated with falls in adults 77 and older (1.67 times the rate), and it is partially reversible with targeted spine and back-extensor work.2
- The Otago Exercise Program (12 weeks of structured strength, balance, and walking work) has the strongest meta-analytic evidence among home-based protocols for improving balance, gait, and lower-limb strength in older adults.5
- If you have already had a fall, take a fall medication, get dizzy when you stand up, or notice your spine has rounded over the past few years, talk to a doctor before starting a self-directed program.
Falls are not random. They are the visible end of a chain that starts in your spine, runs through your hips, and finishes at your ankles. The Centers for Disease Control reports more than 1 in 4 adults aged 65 and older fall each year, accounting for roughly 3 million emergency department visits and 43,000 deaths annually, with both numbers trending up.1 Inside that statistic is a quieter one: most of the risk lives in posture mechanics that a 12-week program can measurably change. This guide walks through the three posture systems that drive fall risk in older adults, the research behind each one, and a week-by-week protocol you can start at home this week.
The numbers behind older-adult falls
More than 1 in 4 Americans aged 65 and older fall each year. The CDC tracks the consequences and the trend is not flattening: about 3 million ED visits annually, roughly 1 million hospitalizations, around 319,000 hip fractures, and more than 43,000 deaths in the most recent reporting year.1 Roughly 37 percent of falls produce an injury serious enough to require medical treatment or restrict daily activity for at least one day. Most older adults who fall once will fall again within twelve months.
These numbers describe outcomes, not causes. The causes split into two buckets: things that are largely fixed (age, sex, sensory decline, certain medications) and things that respond to a few weeks of targeted work (strength, balance, joint range, postural alignment). The fixed bucket is what makes fall prevention feel inevitable. The modifiable bucket is the reason this guide exists.
Inside the modifiable bucket, three posture mechanics carry an outsized share of the risk. Each one is measurable. Each one moves with practice. And each one shifts your center of mass either back toward your base of support (low risk) or further outside it (high risk). Get those three right and you change the input to your nervous system every time you take a step.
Most of the risk lives in posture mechanics that a 12-week program can measurably change.
The three posture mechanics that drive fall risk
Standing upright is a balance act. Your nervous system reads where your center of mass sits, where your feet sense the ground, and how strong the muscles are that pull you back toward neutral when you start to drift. When any one of those inputs degrades, your margin shrinks. When two or three degrade together, falls become the predictable outcome of normal life: stepping off a curb, reaching for a high shelf, turning quickly in the kitchen.
The three posture systems that matter most in older adults are the thoracic spine (specifically the angle of forward curvature), the ankle and foot complex (range of motion and toe strength), and the hip abductor and glute group (lateral stability during walking and single-leg stance). These three were not chosen because they sound related. They were chosen because each one has independent prospective evidence linking it to fall incidence in adults over 65.
The good news is that all three are partially or fully reversible at any age, and the work that targets one tends to improve the others. The protocol later in this post is built around that fact. Before the protocol, here is the mechanism behind each system, so you understand what you are training and why.
Why your thoracic spine controls your balance
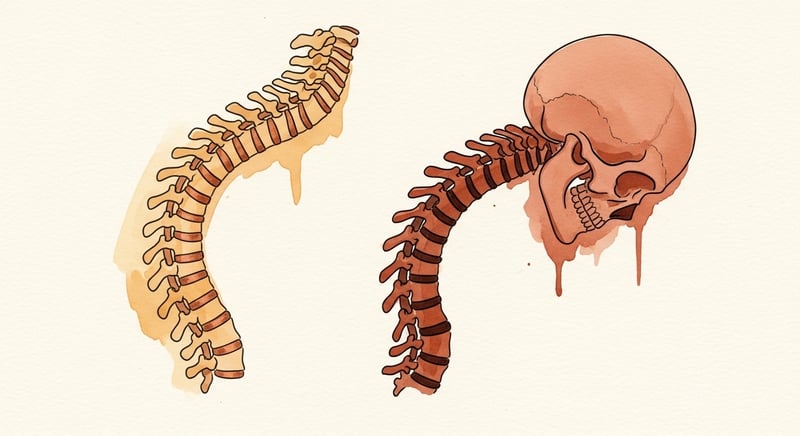
When the upper back rounds forward beyond its natural curve, the head moves ahead of the shoulders, the chest sinks, and the rib cage tips toward the floor. This shift, called hyperkyphosis when the curve exceeds about 50 degrees on a side X-ray, does three things at once: it moves your center of mass forward of your base of support, it reduces the visual field ahead of your feet, and it shortens the distance between your ribs and your pelvis enough to weaken the deep stabilizers that protect you in a stumble.
A 2022 prospective study in Osteoporosis International followed 1,220 community-dwelling older adults for two years. In the overall sample, hyperkyphosis showed no association with falls. But when the researchers restricted the analysis to participants aged 77 and older, hyperkyphosis was prospectively associated with a 1.67-times higher rate of falls.2 The authors explicitly noted that hyperkyphosis is partially reversible and called for it to be tested as a fall-prevention target. For more on the curve itself, the dowager's hump explainer covers the cosmetic-versus-clinical distinction in detail.
Reversibility comes from two sources. The first is muscular: the back extensors (especially the thoracic erectors and middle and lower trapezius) lose strength with age and disuse, and that weakness lets the chest sink forward under gravity. Strengthening them lifts the spine back toward neutral. The second source is mobility: the joints between thoracic vertebrae stiffen in flexion when the position is held for years. Targeted extension drills restore the range. Both responses happen within weeks.
What does NOT reverse with exercise is structural change from vertebral compression fractures or advanced osteoporosis. If you have had a fracture or your spine has rounded suddenly rather than gradually, the work in this post still helps but the program needs to be supervised. The aging and posture overview walks through how to tell the two patterns apart.
The ankle and toe story (the most overlooked piece)
Ask most people what causes falls in older adults and they say balance. They are not wrong, but balance is the symptom, not the cause. The cause is often a few centimeters of lost ankle range and a few pounds of lost toe strength. Together those two changes turn a recoverable wobble into a fall.
A 12-month prospective study in the Journal of Gerontology followed 176 older adults with a mean age of 80. By the end of the year, 41 percent had fallen at least once. The fallers were not weaker overall, and they did not have worse vision or worse cognition than the non-fallers. What separated them, statistically, was decreased ankle flexibility (specifically dorsiflexion range) and decreased toe plantarflexor strength, both of which were independently associated with falls.3 In plain terms: the people whose ankles could not bend forward enough and whose toes could not push down hard enough were the ones who fell.
The mechanism is straightforward. When you walk, your foot strikes the ground heel first. Your ankle dorsiflexes (bends forward) to keep your shin moving over the foot. If that motion is restricted, your gait shortens, your stride asymmetry grows, and your foot loses contact with the ground earlier in each step. At toe-off, your toes need to push the body forward and stabilize the ground transition. Weak toes mean a sloppier push and a less reliable last contact with the floor before swing.
The fix is two-part. Mobility comes from a daily wall calf stretch (back foot heel down, front knee bent, lean into the wall, hold 30 seconds, switch). Strength comes from heel raises (rise onto your toes, hold 2 seconds, lower slowly) and toe-curl drills (towel scrunches with the toes on a bath mat). The protocol in section seven puts these in their place; for now, just notice that ankle and toe work is closer to fall prevention than balance work itself.
If your ankle stiffness is severe (less than 5 degrees of dorsiflexion when tested), that often points upstream to tight calves and posterior-chain restriction. The thoracic spine mobility post covers the upper-back cousin of the same pattern, and many of the principles transfer.

Hip strength: the lateral stability you cannot see
When you walk, every other step is a single-leg stance. Your gluteus medius and minimus on the standing side have to hold your pelvis level while the other leg swings through. If those muscles are weak, the pelvis tips toward the swinging side (a Trendelenburg gait), the trunk leans the opposite way to compensate, and your center of mass drifts laterally outside your base of support. On a flat floor at home, this is invisible. On a curb, a wet sidewalk, or a stair, it becomes the moment the fall starts.
A 2022 systematic review in Archives of Physical Medicine and Rehabilitation analyzed 59 studies covering 2,144 participants across age groups. The authors concluded that greater hip abduction torque capacity is critical during balance and mobility tasks at every age tested, with hip abductor strength specifically associated with better Berg Balance Scale, Y Balance, and Timed Up and Go scores in older adults.4 The lateral hip group is the rotation point that keeps your trunk over your base. Lose strength there and balance becomes work.
The exercises are not complicated. Side-lying leg raises (lying on your side, top leg straight, lift to about 30 degrees, hold a beat, lower slowly) train the gluteus medius directly. Standing hip abductions against a wall or with a light resistance band do the same in a more functional position. Single-leg stance practice (hold a chair lightly, lift one foot, work toward 30 seconds without leaning into the chair) trains the same group dynamically. Two or three sets of ten on each side, four times a week, produces measurable change in eight to twelve weeks.
Hip extensors (the gluteus maximus and hamstrings) matter too, particularly because reduced hip extension during walking is one of the clearest gait differences between healthy older adults and older fallers. Weak glutes lead to a shuffling stride with the pelvis tilted forward, which moves your center of mass forward in the same direction the kyphotic spine pushes it. The two problems compound.
The lateral hip group is the rotation point that keeps your trunk over your base. Lose strength there and balance becomes work.

The 12-week protocol
The strongest evidence for a structured home-based fall-prevention protocol comes from the Otago Exercise Program (OEP), developed in New Zealand and tested across multiple randomized trials over two decades. A 2025 systematic review and meta-analysis of 15 RCTs covering 1,278 participants confirmed that OEP improves balance, gait, and lower-limb strength in older adults, with the strongest effects in those with already compromised health.5 The version below adapts the OEP framework around the three posture systems above.
Weeks 1 to 4: Foundation. The goal of the first month is to build the habit and recover the baseline mobility and strength that age-related disuse has cost you. Sessions are 20 to 30 minutes, three times a week, plus a short daily walk.
Each foundation session includes: 5 minutes of warm-up (marching in place, arm swings, shoulder rolls), wall calf stretch (30 seconds each side, twice), thoracic extension over a rolled towel (5 deep breaths, 3 sets), heel raises (2 sets of 10), seated marching (2 sets of 10 each leg), side-lying leg raises (2 sets of 8 each side), and 30 seconds of single-leg stance with light fingertip support each side. Daily walking adds 10 minutes at conversational pace, working up to 20 minutes by week 4.
Weeks 5 to 8: Progression. The second month adds load and reduces support. Heel raises move to 3 sets of 12, ideally on a step with the heels dropping below the step level. Side-lying leg raises increase to 3 sets of 12 each side. Single-leg stance progresses to 30 seconds without support, then with eyes closed (briefly, near a wall). Thoracic extension moves to 8 to 10 reps per session. Walking extends to 25 to 30 minutes most days, and ideally adds one walk per week on uneven ground (a park path, a quiet trail, anything that requires the ankle to negotiate texture).
Weeks 9 to 12: Integration. The third month integrates the work into balance-challenging combinations and adds a strength block. Sessions move to 30 to 40 minutes, with 10 minutes added for: tandem walking (heel-to-toe, 20 steps), step-ups to a low step (2 sets of 10 each leg), and standing hip abductions with a light resistance band (3 sets of 12 each side). Single-leg stance reaches 60 seconds with light fingertip support and 20 seconds without. Walking holds at 30 minutes most days, with the uneven-ground walk happening twice a week.
What you should notice by the end of week 12: your single-leg stance time should at least double, your dorsiflexion should improve by a few degrees, your thoracic extension should feel measurably less stiff, and walking should feel like the floor is giving you back more energy than it did before. If any of those are not happening, the protocol is too easy or you are missing sessions. Consistency matters more than intensity at this stage.

Home environment and daily habits that compound the protocol
Exercise reduces the rate at which your body becomes a fall risk. Environment reduces the rate at which your home presents the trigger. The CDC's STEADI initiative recommends four parallel actions for older adults at fall risk: talk to a doctor about fall risk and current medications, keep moving with strength and balance work, get vision checked annually, and make the home safer.6 The exercise piece is the longest lever. The other three protect the gains while they accumulate.
Home safety is mostly about three rooms. In the bathroom, install grab bars in the shower and beside the toilet, use a non-slip bath mat, and consider a shower seat if standing for the full shower causes light-headedness. In the bedroom, keep a lamp within reach of the bed, clear the path to the bathroom, and remove throw rugs that slide. On stairs, make sure both rails are firmly anchored, both ends of the staircase are well lit, and any rugs at the top or bottom are taped down. These three changes together cost a few hundred dollars and remove the most common indoor fall locations.
Outside the home, walking surface matters more than walking distance. Two short walks on uneven park ground train your nervous system more than one long walk on a smooth sidewalk. Carry a phone with you on outdoor walks, especially if you live alone. If you use a walking aid (a cane, a walker, hiking poles), have someone qualified check the height and the technique. A cane that is two inches too short or held in the wrong hand can increase fall risk rather than reduce it.
Medications matter too. Several common prescriptions raise fall risk on their own (sleep aids, anti-anxiety drugs, blood-pressure medications that drop standing blood pressure, anticholinergics). Polypharmacy (taking five or more medications) approximately doubles fall risk on its own, regardless of what the medications are. Bring your full list to your next physician visit and ask explicitly which ones might be contributing. The conversation is short and the risk reduction is real.
For more on the daily-habit layer that supports the protocol from morning to night, the posture and daily habits guide covers the small choices that either reinforce or undo the work you are doing in your sessions. The walking posture technique guide covers stride mechanics in more depth than this overview.

When to see a professional
The protocol above is built for adults who are independently mobile, have not had a recent fall with injury, and are not on medications that affect balance. If any of the following apply to you, talk to a doctor or physical therapist before starting a self-directed program. None of these are reasons to give up on the work; they are reasons to do the work with supervision so it is safe.
See a doctor if you have had any fall in the past year that you cannot fully explain, especially if you lost consciousness or hit your head. Recurrent unexplained falls can signal cardiac, neurological, or vestibular problems that exercise alone will not address.
See a doctor if your spine has rounded suddenly rather than gradually over years. Sudden kyphosis change is a red flag for vertebral compression fracture, especially if you have a history of osteoporosis, long-term steroid use, or you are post-menopausal and have not had a recent bone density scan.
See a doctor if you get dizzy when you stand up, especially if you take blood pressure medication. Orthostatic hypotension is treatable, and a pre-existing case will undermine any balance work you try.
Work with a physical therapist if your single-leg stance time is under 5 seconds at the start. That is below the threshold where home practice is safe without supervision, and a few sessions with a PT will set you up for the rest of the program.
Finally, if you are unsure where you stand on any of these, the safest first step is a conversation with your primary care doctor specifically focused on fall risk. The CDC's STEADI initiative gives clinicians a structured screening protocol for exactly this conversation, so the visit will be more productive than a general check-up.6 None of the work in this guide should be done in isolation when there are red flags. With supervision, every part of it remains accessible.
None of these are reasons to give up on the work. They are reasons to do the work with supervision so it is safe.
Frequently Asked Questions
How long before I notice a difference?
Most older adults notice their first measurable change between weeks 3 and 5: longer single-leg stance, less stiffness in the morning, easier time stepping off curbs. Visible posture changes (a less rounded upper back, a more lifted chest) usually take 8 to 12 weeks of consistent work. The Otago Exercise Program data suggests the strongest gains in balance and gait emerge by week 12.5
Can I do this if I have already had a fall?
Yes, with supervision. A previous fall is a strong predictor of future falls, so the work matters more for you, not less. But the entry point should be a physical therapist visit rather than a self-started home program, both to rule out underlying contributors (cardiac, vestibular, neurological) and to set the right starting load. Once you have the green light, the protocol in this post is the framework you can use.
Is the dowager's hump reversible?
Partially, depending on whether the curve is muscular or structural. Muscular kyphosis (postural rounding without bone change) responds well to extensor strengthening and thoracic mobility work and can shift several degrees in 12 weeks. Structural kyphosis from vertebral compression fractures cannot be fully reversed because the bone shape has changed, but the surrounding muscles can compensate and slow further progression. The dowager's hump explainer covers how to tell which one you have.
Do I need equipment?
No. The full 12-week protocol uses a wall, a chair, a step (or the bottom stair), and optionally a light resistance band. None of those cost more than a few dollars together. The Otago Exercise Program was designed specifically to work in the home with minimal equipment, which is part of why it has the largest evidence base for community-dwelling older adults.
What if I cannot do single-leg stance at all?
Start with double-leg stance with eyes closed, working toward 30 seconds without swaying significantly. From there, progress to a narrow base (heels touching, toes apart), then heel-to-toe stance (one foot directly in front of the other), then single-leg stance with both hands on a counter. Each progression typically takes 1 to 2 weeks. If you cannot achieve any of these safely, see a physical therapist before continuing.
Are posture correctors helpful for kyphosis?
They can give a temporary reminder of upright position, which some older adults find useful for the first few weeks of habit formation. But correctors do not strengthen the back extensors, do not improve thoracic mobility, and stop working the moment they come off. The research evidence for sustained kyphosis change comes from exercise, not from bracing. The posture corrector evidence post covers what the studies actually show.