Plantar Fasciitis and Posture: An Upstream View
Key Takeaways
- Plantar fasciitis affects about 1 in 10 adults at some point in life, drives roughly 1 million US doctor visits per year, and most often shows up in working adults aged 25 to 65.2
- The single strongest mechanical risk factor is reduced ankle dorsiflexion (how far your shin can bend forward over a planted foot). Tight calves drive that restriction.3
- A 2021 study in Foot and Ankle International found a strong correlation (R = 0.76 to 0.78) between gastrocnemius tightness and heel pain severity. The tighter the calf, the worse the morning first-step pain.1
- Treating only the foot (rolling, ice, anti-inflammatories) often relieves symptoms short term and lets the same condition return in months. Treating the calf-Achilles-fascia chain reduces recurrence.
- About 90% of plantar fasciitis cases respond to consistent conservative treatment within 6 to 8 weeks. Most of that work is upstream of the heel.4
Heel pain that bites on the first step out of bed is the most common signature of plantar fasciitis, and it is also the symptom that sends most people looking for a foot solution. The foot is the wrong place to look first. Decades of evidence point upstream, to the calf and the ankle, as the part of the chain that decides whether the plantar fascia is overloaded or properly supported. This post walks through why that is, how to test for the upstream restriction yourself, and what to do about it before reaching for the next pair of inserts.
Why most heel-pain treatment misses the upstream cause
Plantar fasciitis is the most common cause of heel pain in adults. About 10% of the general population experiences it at some point, and 83% of those affected are active working adults between the ages of 25 and 65.2 The classic presentation is sharp pain at the inside-front of the heel that is worst on the first few steps of the morning, eases as you walk around, and returns after long periods of sitting or after long days on your feet.
The standard advice tends to start at the foot: stretch the fascia, roll a frozen bottle under the arch, try a night splint, get a better insole. All of those have evidence behind them. But the most consistent finding in the modern literature is that the strongest single mechanical driver of plantar fasciitis is not the foot itself. It is restricted ankle dorsiflexion (the inability of the shin to bend forward over a planted foot through enough range), and the tight calves that produce that restriction.3
When the calf is tight, the ankle cannot achieve enough dorsiflexion during the second half of the gait cycle. The body has to find that lost range somewhere else. Most often it finds it by collapsing the arch and over-pulling on the plantar fascia at heel-strike and toe-off. Every step becomes a small overload on the same tissue. Over weeks and months, that overload accumulates into the morning sharp pain people associate with plantar fasciitis.
This is why a foot-only treatment plan often relieves the symptom for a few weeks then watches it return. The fascia calms down, but the upstream restriction that overloaded it has not changed, so the same overload starts again the moment activity resumes. Treating the calf and the ankle is the part most foot-only protocols leave on the table.
The strongest single mechanical driver of plantar fasciitis is not the foot itself. It is restricted ankle dorsiflexion.

The calf-Achilles-fascia chain
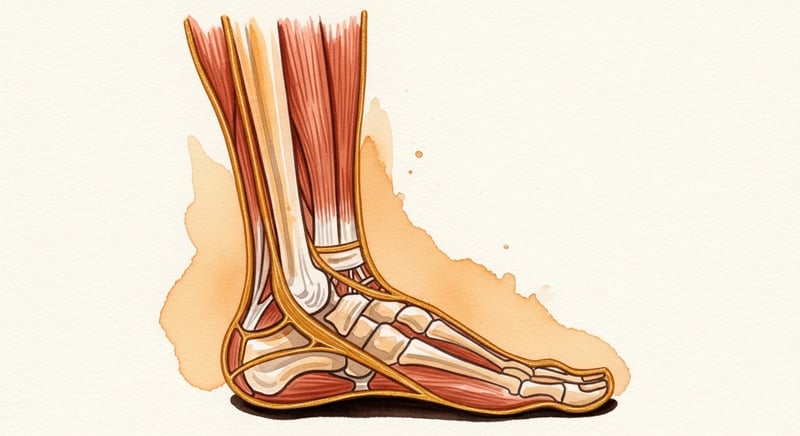
The clinical name for the connection is the posterior chain of the lower leg. Anatomically, the gastrocnemius and soleus (the two layers of the calf) blend into the Achilles tendon at the back of the heel. The Achilles attaches to the back of the calcaneus (heel bone). On the underside of that same heel bone, the plantar fascia originates and runs forward as a thick fibrous sheet to the base of the toes. Mechanically, the calf, the Achilles, and the fascia are continuous. A pull on one end is felt at the other.
A 2021 prospective study in Foot and Ankle International measured this directly. The researchers used a standardized clinical test to quantify gastrocnemius tightness in patients with plantar fasciitis, then correlated those measurements against the patients' pain on the first steps of the morning and their worst pain throughout the day. The correlation was strong: R = 0.757 for first-step pain and R = 0.781 for worst pain (P < 0.001 for both).1 In plain language, the tighter the calf, the worse the heel pain. Across the cohort, calf tightness explained more than half of the variance in pain severity.
The mechanism the study points to is the one above: tight calves restrict ankle dorsiflexion, the foot has to find the missing range somewhere else, the plantar fascia takes the load. The implication is direct. If you can restore ankle dorsiflexion (which usually means lengthening the calf), the load on the fascia drops, and the tissue gets a chance to recover.
The same principle is why running coaches have started flagging calf flexibility as a marker for plantar fasciitis risk in athletes long before the pain shows up. The literature on this group is consistent: calf tightness is one of the more reliable warning signs. The companion principle, that proximal posture also influences foot mechanics, applies in some cases (overpronation linked to internal hip rotation, for example), but the calf-and-ankle axis carries the most consistent evidence as the primary upstream driver.
Two reliable self-tests
Two tests, both quick, both useful at home.
The knee-to-wall test for ankle dorsiflexion. Stand barefoot facing a wall. Place your big toe a measured distance from the wall (start with 4 inches, about 10 cm). Keep your back heel on the floor. Try to touch your knee to the wall. If you cannot, your dorsiflexion is below the working range that healthy walking on uneven ground requires. A normal-functioning ankle should reach the wall with the toe at 4 to 5 inches; a stiff ankle struggles past 2 to 3 inches. Test both sides. Asymmetry is its own warning sign even when both sides reach a similar number.
The first-step pain rating. When you wake up and put your weight on your heel for the first time, rate the pain from 0 (no pain) to 10 (worst imaginable). Track the number for two weeks. The 2021 calf-tightness study used the morning first-step pain rating as the primary outcome variable because it is the most reliable marker of whether the fascia is recovering or staying inflamed.1 If the number is trending down across consistent treatment, you are on track. If it is plateaued or rising, the program is not addressing the upstream restriction.
Together these two tests tell you both what the restriction is (knee-to-wall) and how the fascia is responding (first-step pain). You do not need imaging or a clinic visit for either.

The upstream protocol
The protocol below targets the calf-Achilles-fascia chain, not just the foot. It is what the modern conservative-treatment literature converges on, and it is what the 90% recovery rate within 6 to 8 weeks comes from.4 Daily, two sessions if you can.
Calf stretch (gastrocnemius), 30 seconds each side, 3 sets. Stand facing a wall, hands on the wall at chest height. Step one foot back, keep the back heel down, back leg straight, front leg bent. Lean into the wall. Hold the stretch where you feel it in the back of the upper calf. Switch sides. This targets the gastrocnemius specifically, which is the part of the calf with the strongest correlation to plantar-fasciitis severity.
Soleus stretch, 30 seconds each side, 3 sets. Same setup but bend the back knee while keeping the heel down. The bend takes the gastrocnemius out of the stretch and isolates the deeper soleus. People often skip this one and miss half of the calf-tightness picture.
Heavy-load slow heel raises, 3 sets of 12 each side, every other day. Stand on the edge of a step with the front of your foot on the step and the heel hanging off. Slowly rise up onto your toes (3 seconds), pause at the top (1 second), slowly lower the heel below the step level (3 seconds). The slow eccentric loading is what the modern Achilles and plantar-fascia rehab evidence consistently supports. Add light hand weights once the bodyweight version becomes easy.
Foot intrinsics: short-foot exercise, 10 reps each side, daily. Sit with bare feet flat on the floor. Without curling the toes, try to draw the ball of the foot back toward the heel by activating the small muscles in the arch. The arch should rise slightly. Hold 5 seconds, release. Strengthens the muscles that actively support the arch and reduces the load the plantar fascia carries passively.
Plantar fascia stretch (still useful, just not the whole answer), 30 seconds each side, 3 sets. Sit. Cross the affected foot over the opposite knee. Pull the toes back toward the shin with the hand. Hold. The fascia stretch is the standard foot-only intervention; it works better when the upstream calf work is also happening.
Most people start to notice the morning first-step pain trending down within 2 to 3 weeks of consistent practice. By week 6 to 8 the majority of cases are substantially improved. If the text neck syndrome post walked through the upstream-versus-downstream pattern for the cervical spine, this is the same logic applied to the foot. The body works as a chain. Treat the chain.
Treating only the foot relieves the symptom. Treating the calf-Achilles-fascia chain reduces recurrence.

When standard treatment isn't enough
About 90% of plantar fasciitis cases respond to consistent conservative treatment within 6 to 8 weeks.4 The other 10% need more help. If any of the following apply to you, talk to a clinician.
See a doctor if your morning first-step pain has not improved after 8 weeks of consistent daily upstream work. At that point you may have one of the less-common drivers (a partial fascia tear, calcaneal stress fracture, tarsal-tunnel-style nerve compression) that home treatment will not address, and imaging is appropriate.
See a doctor if your heel pain came on suddenly with no warning rather than building gradually. Sudden-onset heel pain, especially after a misstep or impact, raises the index of suspicion for a partial fascia tear or stress reaction.
See a doctor if you have any numbness, burning, or tingling in the heel or arch. That pattern points to nerve involvement (most often the medial calcaneal branch of the tibial nerve) rather than fasciitis, and the treatment is different.
See a doctor if you have diabetes and you are starting any foot pain protocol. Diabetic neuropathy can mask the warning signs that protect the foot, and the standard protocol may need to be modified. The back-pain post covers a parallel logic for the lumbar spine, where home work is appropriate for most people but specific risk factors warrant professional input first.
Frequently Asked Questions
Why is plantar fasciitis worse in the morning?
While you sleep your foot rests in plantar flexion (toes pointed slightly down), which lets the plantar fascia and the Achilles tendon shorten. The first weight-bearing step of the morning suddenly stretches both, and the inflamed fascia tears at the micro level again. By a few minutes of walking the tissue has warmed up and the pain eases, until the next long rest.
Do I need orthotics?
Sometimes. Custom orthotics can help in cases with significant pes planus (flat feet) or pes cavus (high arches) that contribute to abnormal load on the fascia. For most cases of plantar fasciitis, however, an over-the-counter arch-supporting insole plus the upstream calf-and-ankle work in this post is enough. Orthotics on their own (without addressing the calf) treat the same symptom-only logic that lets the condition recur.
Are night splints worth it?
Yes for some people. A night splint holds the ankle in slight dorsiflexion overnight, preventing the calf and fascia from shortening while you sleep. The morning first step lands on tissue that is already stretched, so the sharp pain reduces. Harvard Health lists night splints as one of the conservative interventions that 90% of cases respond to.4 They are most useful for people whose morning first-step pain is the dominant symptom and whose daytime symptoms are mild.
Should I run with plantar fasciitis?
Yes if morning first-step pain is below about 4 out of 10 and trending down. Drop mileage by 30 to 50%, shift to softer surfaces (grass, dirt, treadmill), and add the calf-and-ankle work as a daily non-negotiable. If first-step pain rises, drop further; if it falls, hold the new volume for two weeks before adding back.
How long does plantar fasciitis take to fully resolve?
About 90% of cases respond to consistent conservative treatment within 6 to 8 weeks.4 Full resolution typically takes 3 to 6 months in moderate cases. Recurrence rates are lower for people who keep the calf and Achilles work as a long-term habit, not just during the symptomatic period.